Reciprocal IVF: About, Timeline, Costs, and More

Reciprocal IVF, also referred to as co-maternity, is a fertility treatment option for lesbian (or trans men) couples that allows both partners to be intimately involved in the child creation process. Since it is not yet possible to create a child by combining two eggs, reciprocal IVF may just be the coolest way to make a baby.
While reciprocal IVF is a great family-building option for those in the LGBTQ community, there’s lots to consider when choosing a fertility treatment that is right for you and your family. In this article, we’ll break everything down from how reciprocal IVF works, costs, insurance coverage, success rates, treatment alternatives, and how to decide who is the ideal partner to carry and whose eggs to use.
Let’s get started with some high-level facts.
Fast Facts About Reciprocal IVF
What is Reciprocal IVF
Reciprocal IVF is a variation of the standard in vitro fertilization procedure where the embryos are made using Partner A’s eggs but are put inside of Partner B’s uterus to carry the pregnancy. That means Partner A (the egg donor or genetic mother) is genetically related to the child, and Partner B (the carrier or birth mother) is biologically bonded to the child through pregnancy.
Does insurance cover reciprocal IVF?
Reciprocal IVF is most often not covered by insurance. Only 25% of Americans have coverage for IVF, and most plans do cover IVF require many failed IUIs before they cover IVF.
What does Reciprocal IVF Cost
Reciprocal IVF costs anywhere from $5,500 to over $30,000, with an average cost of over $20,000 in the United States. The cost of reciprocal IVF is incredibly variable and depends on:
- the clinic
- medication protocols
- add on services like genetic testing or sex/gender selection
Fortunately, there are financing options available to many.
Key Questions to Answer Before Starting
Before starting a co-maternity IVF cycle, it’s important to know:
- whose eggs you will use
- whose will carry the pregnancy
- whose sperm you will use
While these decisions may be entirely personal, it is often steered by fertility testing and the guidance of a fertility doctor to determine what gives you the best odds of success.
Key Terminology
- Co-Maternity – reciprocal IVF synonym
- Egg Donor, Genetic Mother, Genetic Parent – Terms used to describe the partner who will be genetically related to the child via their eggs. This “egg donor” is not to be confused with an anonymous egg donor.
- Carrier, Birth Mother, Birth Parent – the partner who will carry the pregnancy
- Egg Retrieval – The egg retrieval is the procedure done to remove the eggs from the genetic parent.
- Embryo Transfer – The embryo transfer is the procedure to transfer the early-stage embryos into the carrier
- Monitoring – Monitoring is the office appointments to check on the egg donor’s follicular and egg development and the carrier’s uterine lining. The baseline is the first monitoring appointment.
How Does Reciprocal IVF Work?
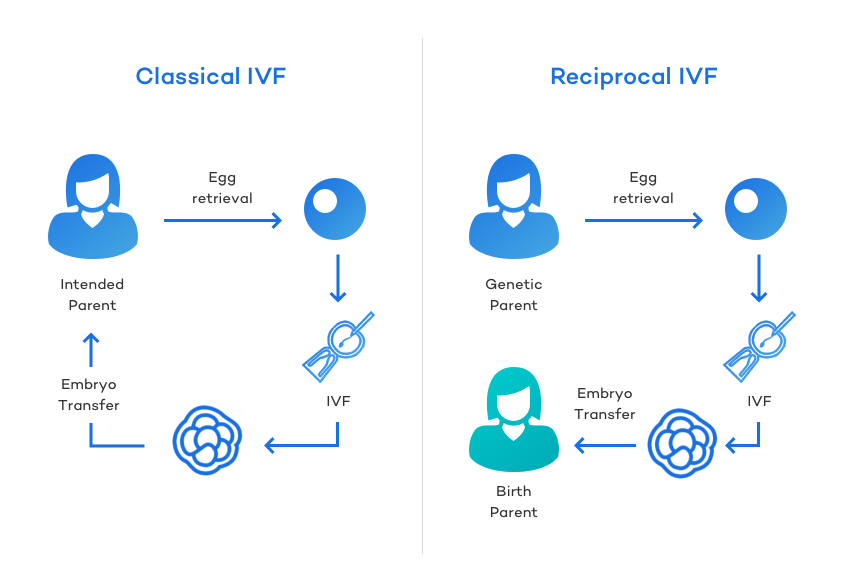
Reciprocal IVF works similar to a standard IVF procedure, but the resulting embryo(s) are placed into their partner’s womb.
Traditional IVF has four main steps. Co-maternity has one additional step before starting the primary IVF process.
- Syncing Cycles (the additional step)
- Ovarian Stimulation
- Egg Retrieval
- The Embryology Lab: Fertilization and Embryo Development
- Embryo Transfer
Syncing Cycles:
To accurately time the embryo transfer, the carrier’s cycle must be synced to the donor’s cycle. While it is true this isn’t necessary if doing a frozen embryo transfer, it is often recommended to try a fresh transfer first with reciprocal IVF (primarily due to cost as the outcomes of fresh and frozen transfers are equivalent in reciprocal IVF but fresh are less expensive), though a frozen transfer may be slightly more convenient for the intended parents.
Why do the cycles need to be synced for a fresh embryo transfer? The cycles need to be synced to ensure that the uterine lining is at the proper stage of development/thickness when the embryo is ready to be transferred. Remember, in “nature” sperm and eggs are meant to meet in the fallopian tubes around day 14-16 of a woman’s menstrual cycle and make it’s way back down to the uterus to implant into the endometrial lining around day 20. That means we want the woman who will be carrying the child to be around cycle day 20 at the same time the embryos are five days old. To ensure that, everything must be aligned from the beginning.
The birth control pill will be used to synchronize the two partners’ cycles. After the cycles are synced, the main part of the treatment can begin.
Ovarian Stimulation (Egg Donor) & Lining Preparation (Carrier):
The Egg Donor:
The simple idea of ovarian stimulation is to take medications for around ten days to encourage more than one egg to mature fully. The hope is that more eggs = more embryos = more/higher chances at a successful pregnancy (remember if you have more than one embryo, the additional embryos can be frozen for future use in case the first transfer fails or for a second child after successfully giving birth).
Ovarian stimulation typically begins on days 2-4 of a woman’s cycle after a baseline appointment to designate the follicular, and hormonal baseline.
This process is followed closely with monitoring appointments every few days to track follicular development and time the egg retrieval procedure. When the follicles reach a specific size (as detected with ultrasound), they are ready for the egg retrieval procedure.
The Carrier:
During this time, the carrier will take estrogen and later progesterone to thicken the lining in preparation for embryo transfer. A thick healthy lining helps the embryo stick and results in higher odds of pregnancy. While it is possible to forego medications, it is usually not recommended.
Though slightly less often than the donor, the carrier will have multiple monitoring appointments to ensure proper lining development.
Egg Retrieval
The egg retrieval is precisely like it sounds. It is a minor outpatient procedure done to collect the developed eggs from the woman’s ovaries so that they can be fertilized in a laboratory. During the procedure, the physician uses a tiny hollow needle with suction capabilities to drain the fluid from the follicles, which contain the developed eggs.
The number of eggs retrieved will depend on your age, history, fertility diagnosis, medication protocol, and response to medications.
The Embryology Lab: Fertilization and Embryo Development
After being retrieved, the eggs are combined with sperm in a petri dish or injected directly with the sperm using an embryonic procedure called ICSI.
After fertilizing, the embryos are grown in nourishing media that mimics the internal environment of a fallopian tube (where early embryonic development naturally occurs), usually for 3-5 days.
If an embryo is grown to a blastocyst stage (typically reached on day 5), it can then be genetically tested. Genetic testing may not be recommended for everyone, but it does give the option for sex/gender selection, helps reduce the risk of miscarriage for some, and can be a useful tool at screening embryos affected by genetic disorders.
Embryo Transfer
An embryo transfer is a minor “procedure” that requires no anesthesia and lasts only a few minutes from start to finish. During an embryo transfer, one or two embryos are gently placed into the carrier’s uterus using a sterile catheter. If the embryo sticks, pregnancy results.
Any embryos that develop to a cleavage or blastocyst stage can be frozen and used for a subsequent Frozen Embryo Transfers. For a frozen embryo transfer, the donor partner would not need to do anything.
Reciprocal IVF Timeline
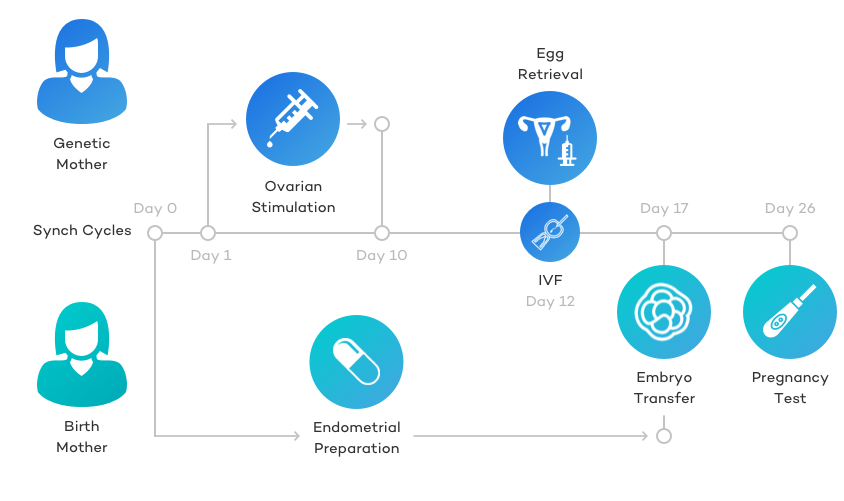
The timeline for a reciprocal IVF cycle can follow two different timelines depending if you want to do a fresh transfer or a frozen transfer.
A fresh transfer uses embryos that have never been frozen. A frozen transfer uses embryos that have been frozen and then thawed, which doesn’t sound that great, but surprisingly results in nearly just as high of success rates (and is often logistically easier).
Reciprocal IVF Timeline With a Fresh Transfer
Fresh transfers are preferred by a very slim margin for doing reciprocal IVF and are generally done unless both partners are not available during the same cycle or if they want to do genetic testing (which requires a FET as it takes time to get the results back).
Overall, a fresh transfer co-maternity IVF cycle lasts around 17 -20 days (excluding the time spent the carrier spends on birth control to sync the cycles) and the ten(ish) days after the embryo transfer waiting for the pregnancy test.
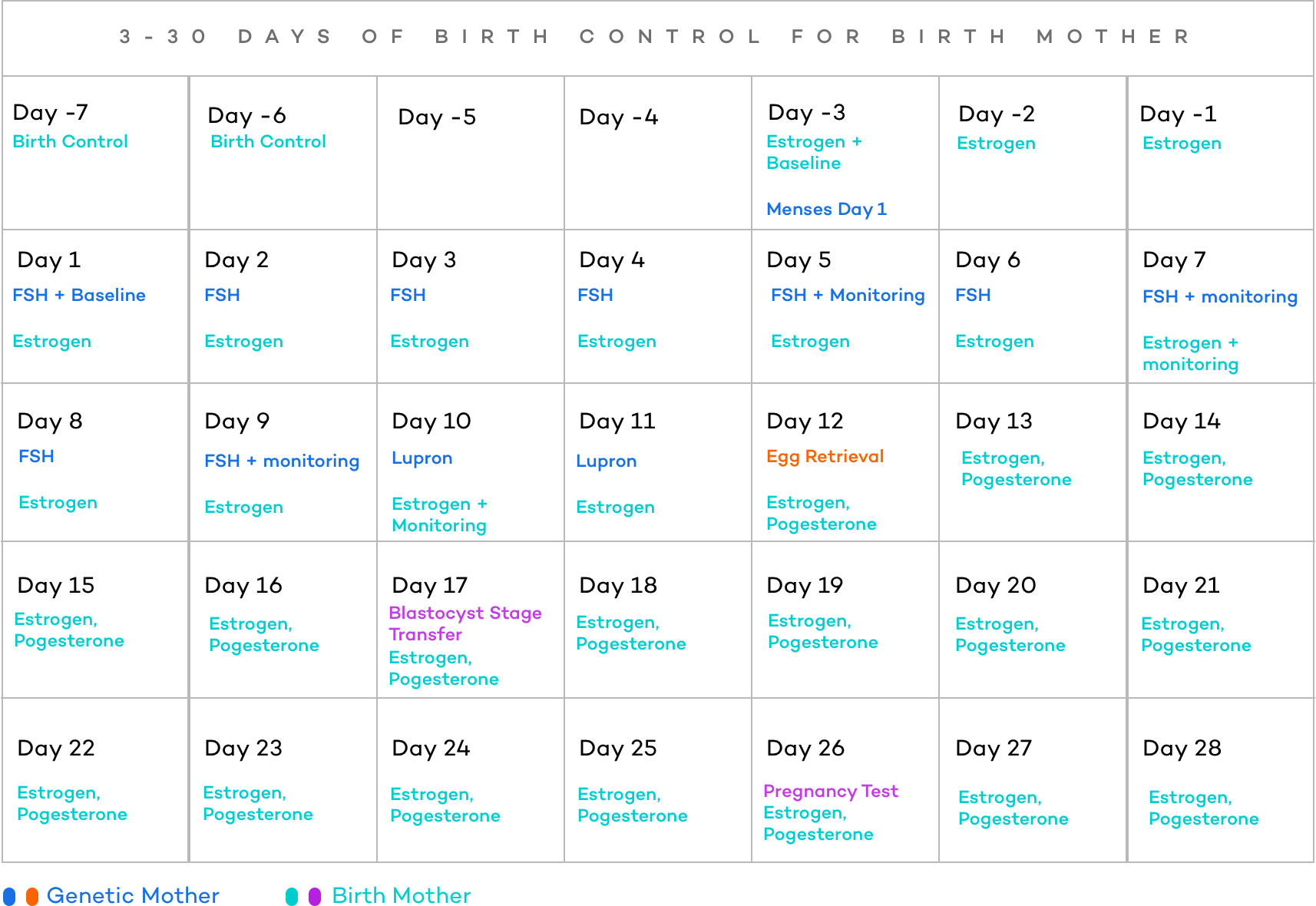
Reciprocal IVF Timeline With a Frozen Transfer
During a Frozen Embryo Transfer Reciprocal IVF Treatment, one of the cycles is fully dedicated to the genetic mother while the carrier does nothing. The second cycle is dedicated strictly to the carrier. The actual time it takes to complete the entire treatment depends on how the menstrual cycles of the two intended parents line up. The FET cycle can be started the first cycle the carrier has after the embryos are frozen. Because reciprocal IVF with an FET takes two cycles, the time to pregnancy is greater (about twice as long assuming both are successful on the first transfer).
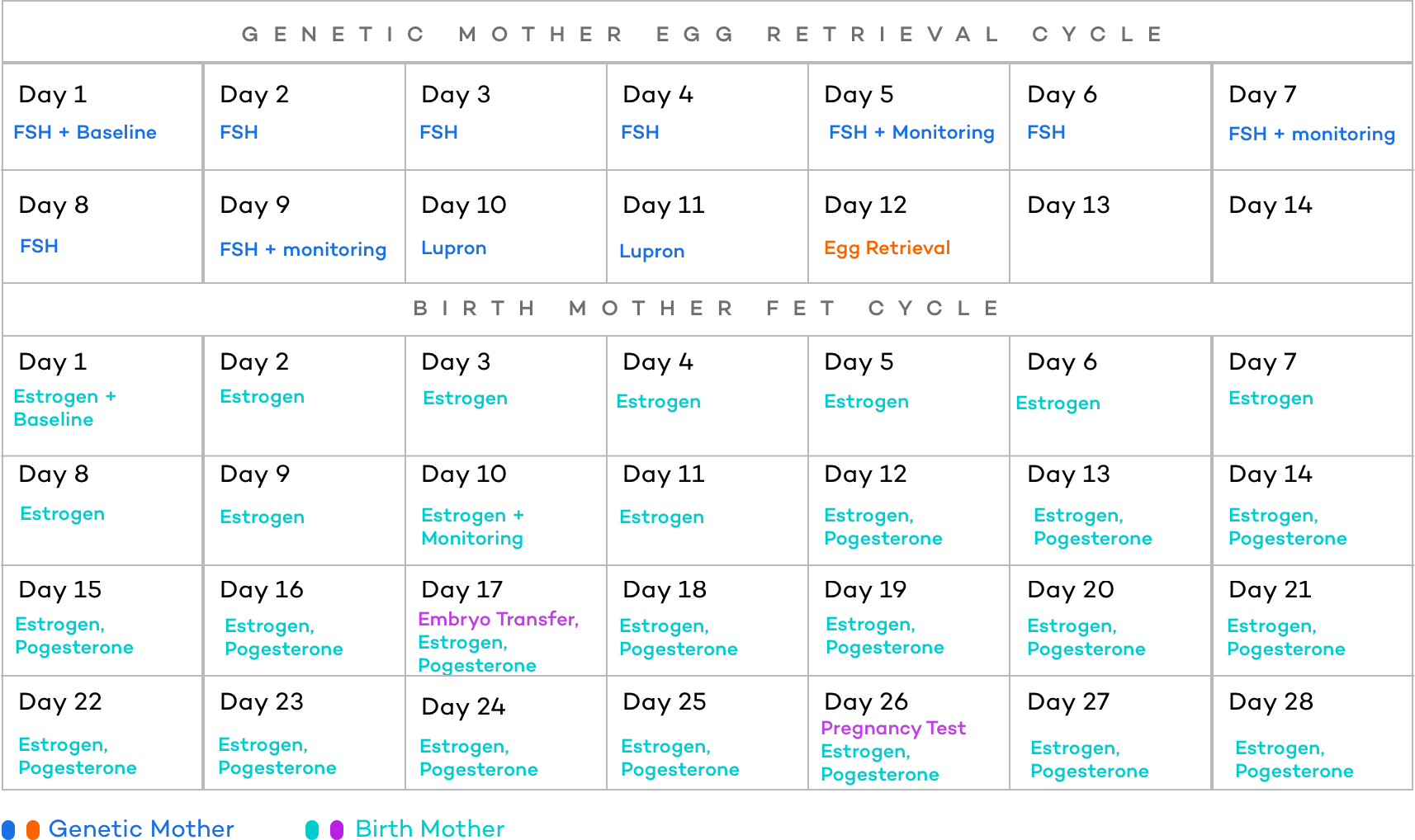
Given the extra time, why might someone do a FET?
Frozen transfers are done for a number of reasons:
- After a failed reciprocal IVF cycle with a fresh transfer
- After a successful fresh or frozen transfer and the desire to grow your family after your first child is born
- In order to do genetic testing to improve the odds of a transfer, avoid potential genetic disorders, or choose the sex of the child
- If both partners are not available during the same cycle
Reciprocal IVF Cost
The cost of reciprocal IVF varies remarkably depending on the fertility clinic, medication protocol, and the addition of add on services like genetic testing. However, given the overall lack of IVF insurance coverage and the average cost of IVF is over $20,000, it’s going to be a fairly pricy procedure any way you slice it. That said, there are significantly more affordable options out there (like here at CNY) so it can pay big time to shop around and potentially travel for treatment. There are also a growing number of states and employers offering coverage so it’s important to check your plan carefully and call your insurance company directly to check on coverage. Who knows . . . you could be one of the lucky 25% with IVF coverage .
Generally speaking, reciprocal IVF will be slightly more expensive than traditional IVF for three main reasons:
- It requires donor sperm (of course, this cost will always be encountered for anyone doing reciprocal IVF)
- Requires both partners to have monitoring appointments
- Requires either 1) more logistics due to cycle syncing or 2) a frozen embryo transfer.
Reciprocal IVF Cost Comparison: CNY Fertility Vs. National Average
Automatically Included
-
{{ tick.item }}
Sample Payment Calculator: Self Pay Pricing
-
{{getTreatmentName()}} {{ treatment_price_discount|toCurrency }}
National Average {{ this.treatment_price_others|toCurrency}} -
{{ treatment.data.price.monitor.remote.label }} Remote Cycle Management {{ total_monitor.cny | toCurrency }}{{ treatment.data.price.monitor.in_house.label }} In House Monitoring {{ total_monitor.cny | toCurrency }}{{ treatment.data.price.monitor.remote.note_calc | stripHTML }} {{ treatment.data.price.monitor.in_house.note_calc | stripHTML }} Third-party fixed fee (SAMA) Third Party {{ total_monitor.others | toCurrency }}{{ treatment.data.price.reciprocal_ivf.note_calc || "Reciprocal IVF requires both partners to be monitored" }} {{ treatment.data.price.frozen_transfer.note_calc_monitor || "" }}
-
-
{{ treatment.data.price.frozen_transfer.label }} Frozen Transfer {{treatment.data.price.frozen_transfer.cny|toCurrency}}
-
{{ treatment.data.price.cryo_preserve.label }} Cryopreservation + 1yr Storage {{treatment.data.price.cryo_preserve.cny|toCurrency}}{{treatment.data.price.cryo_preserve.note_calc | stripHTML}} Third Party {{treatment.data.price.cryo_preserve.others|toCurrency}}
-
{{ treatment.data.price.genetic_testing.label }} Genetic Testing {{treatment.data.price.genetic_testing.cny|toCurrency}}{{treatment.data.price.genetic_testing.note_calc | stripHTML}} Third Party {{treatment.data.price.genetic_testing.third_party|toCurrency}}
-
{{ treatment.data.price.medication.label }} Medication Estimate {{total_medication.cny|toCurrency}}{{total_medication.note_calc | stripHTML}} Third Party {{total_medication.third_party|toCurrency}}
-
{{ treatment.data.price.medication.label }} Medication Estimate {{total_medication.cny|toCurrency}}{{total_medication.note_calc | stripHTML}} Third Party {{total_medication.third_party|toCurrency}}
-
{{ treatment.data.price.zymot.label }} ZyMōt Sperm Processing ${{treatment.data.price.zymot.cny}}{{ treatment.data.price.zymot.note_calc | stripHTML}} Third Party ${{treatment.data.price.zymot.third_party}}
-
{{ treatment.data.price.pregmune.label }} Pregmune Reproductive Immunology Testing {{treatment.data.price.pregmune.cny|toCurrency}}{{ treatment.data.price.pregmune.note_calc | stripHTML}} Third Party {{treatment.data.price.pregmune.third_party|toCurrency}}
-
{{ treatment.data.price.donor_eggs.label }} Donor eggs {{total_donor_eggs.cny|toCurrency}}{{treatment.data.price.donor_eggs.note_calc | stripHTML}} Third Party {{total_donor_eggs.others|toCurrency}}
-
{{ treatment.data.price.donor_sperm.label }} Donor sperm {{treatment.data.price.donor_sperm.cny|toCurrency}}{{treatment.data.price.donor_sperm.note_calc | stripHTML}} Third Party {{treatment.data.price.donor_sperm.others|toCurrency}}
-
{{ treatment.data.price.donor_eggs.label }} Donor Package {{total_donor_package.cny|toCurrency}}{{treatment.data.price.donor_package.note_calc | stripHTML}} Third Party {{total_donor_package.others|toCurrency}}
-
{{ treatment.data.price.gestational_surrogacy.label }} Gestational Surrogacy {{treatment.data.price.gestational_surrogacy.cny|toCurrency}}{{treatment.data.price.gestational_surrogacy.note_calc | stripHTML}} Third Party {{treatment.data.price.gestational_surrogacy.others|toCurrency}}
-
{{treatment.data.price.split_cycle.label ? treatment.data.price.split_cycle.label : "Split Cycle Discount" }} {{discount_split_cycle|toCurrency}}
-
5% Military & Veteran Discount {{discount|toCurrency}}
-
Installments Fee {{finance.fee|toCurrency}}
-
Total to CNY {{total.total | toCurrency}}
Estimated 3rd Party Costs {{total.third_party| toCurrency}}
Grand Total {{(total.total + total.third_party)| toCurrency}}
National Average: {{total.national|toCurrency}} -
Down Payment to CNY{{finance.payment_down_amount|toCurrency(2)}}
-
Monthly Payment to CNY{{finance.monthly_payment|toCurrency(2)}}
{{ treatments[treatment_selected]['data']['footnote'] }}
The above calculation is for simulation purposes only. It is reflective of self-pay pricing, includes highly variable estimates paid to CNY and third parties, and national averages obtained through internal research, FertilityIQ, ASRM, and Resolve. Billing through insurance will likely result in substantially different fees. CNY Fertility does not warrant or guarantee any price for services conducted or rendered by a third party and recommends everyone obtain written estimates from any medical facility involved in your treatment as well as verification of coverage from your insurance company prior to beginning treatment.
1 USD = {{currency.rates[currentCurrency]}} {{currentCurrency}}
Last Update {{currency.last_update}}
Now that you’ve played around with our reciprocal IVF pricing calculator a little let’s explore each of the potential line item costs in closer detail.
Base IVF Package
What exactly constitutes a base package differs greatly from clinic to clinic. Here at CNY it includes:
- The egg retrieval and associated anesthesia
- Conventional or ICSI fertilization
- One Fresh Embryo Transfer
It doesn’t include monitoring or medications – both of which are essential in just about every scenario, but are left out of our base package because 1) many people travel to us from out of the area and have their monitoring done locally that way they only have to be away from home for a short 2-7 days and 2) medications are billed for directly by the pharmacy. Just as we at CNY do not include monitoring or medications in our prices, it is very common for other clinics to break their services down into line items and bill separately for them. Medications will never be included in a clinic’s cost.
Our base IVF package cost $3,900 – with monitoring it is $4,700. This is compared to a national average of around $13,500.
Learn more about the cost of IVF and all it’s variable components here.
The Cost of Donor Sperm
Donor sperm can come from a known donor or it can be purchased from a sperm bank for a price of approximately $750.
Additional Costs Specific to Reciprocal IVF
As mentioned reciprocal IVF requires a few extra costs than conventional IVF.
Additional Monitoring:
In order to do reciprocal IVF, both partners must be monitored. Here at CNY monitoring is $800 for the genetic parent and $950 for the birth parent.
Cycle Syncing or FET:
While CNY doesn’t charge extra for cycle syncing, many clinics will. Every clinic will charge for a FET should you choose to go that route (or need more than one transfer). The price for a frozen embryo transfer ranges greatly from about $650 (plus monitoring and medications) here at CNY, but on average costs around $4,000 (plus monitoring and medications)
Genetic Testing
Genetic testing is a fee not encountered by everyone, but may be used to help select a genetically normal embryo to transfer or to choose the sex of the child.
Concerns Regarding Cost
Cost per treatment vs. cost per birth:
One important distinction not often covered by fertility clinics is the potential difference in the cost of one treatment vs. the cost to bring home a baby. The unfortunate reality is that IVF doesn’t always work.
One study suggests that the “average couple” will need 2 IVF cycles in order to bring home their baby.
Other Options:
Because the cost of reciprocal IVF is cost-prohibitive for many, some couples look at potentially more affordable options like IUI (AKA artificial insemination) before proceeding onto IVF or reciprocal IVF.
That said, it’s important to remember that although IUI is less costly on a per treatment basis, the cost of an IUI isn’t always less on a per birth basis. Because of this, it’s important to have your testing completed and consultation with your fertility specialist prior to making a decision to proceed with any fertility treatment.
Reciprocal IVF Insurance Coverage
Unfortunately, there is little insurance coverage for reciprocal IVF. In fact, only eight states mandate IVF coverage in some form, and many of those states have a significant number of exemptions leaving many without coverage. According to resolve, most states that require IVF coverage also require a certain number of failed IUI attempts or medical diagnosis that would make IUIs futile.
Besides states that mandate fertility coverage, there are a significant number of companies now expanding their fertility treatment coverage as a way to attract and maintain a talented workforce.
Reciprocal IVF Financing
Because reciprocal IVF is such an attractive family building option for many in the LGBTQ community but is cost-prohibitive to many, a large number of people pursuing reciprocal IVF turn to a one or more options for financing. Financing for reciprocal IVF is offered through a number of different institutions:
Fertility Clinic Payment Plans:
Most fertility clinics (or all but one fertility clinic, us, here at CNY Fertility) shy away from being both the treatment provider and “lender.” CNY Fertility payment plans allow everyone, yes, everyone, the ability to pay for their treatment over 24 months. The pros of CNY payment plans is that they are operated by the fertility clinic offering the treatment, have a 100% approval rating without even a credit check, and have a reasonable financing fee. Some cons would be the lack of financing for things like medications or other expenses paid to third parties and the fact that it is only available if your treatment is done at CNY.
Lending Companies and Banks:
Loans from fertility lending companies and banks are varied and diverse and include:
Fertility Lending Companies:
Often partner with specific clinics to offer financing in partnership with that clinic. The good thing is you can get funding past fertility clinic bills and often apply with the fertility clinic, but credit restrictions apply, and financing may only be available at certain clinics.
Personal Loans:
Personal loans from banks or credit unions offer lower interest rates than your average credit card and can be a good option, particularly if you have an existing relationship. Lenders often require good credit.
Grants:
While technically not financing, many fertility clinics and organizations offer grants as a way to offer free or discounted IVF. Rules and application requirements vary greatly, so you’ll want to do your research.
Who should do reciprocal IVF?
In short, Reciprocal IVF may be a great family-building solution for lesbian couples and pre-transition men. Generally speaking, those who pursue reciprocal IVF do so because they either:
- Failed lesser treatments like IUI (or have a fertility diagnosis contraindicative of lesser treatments) and must face the higher cost of IVF regardless so choose to do reciprocal IVF because . . . why not?
- Absolutely love the idea of both being biologically connected to the child creation process either through genetics or pregnancy and choose to skip lesser treatments.
Of course, there is a relatively rare situation in which one partner makes an excellent egg donor but is truly unfit to carry a pregnancy or visa versa, but most decisions of pursuing reciprocal IVF are made for one of the two reasons.
Double Reciprocal IVF
Some couples doing reciprocal IVF choose to both go through both parts of the reciprocal IVF process at the same time. That means Partner A and Partner B simultaneously take stimulation medications and egg retrieval, and transfer the other’s embryo into them.
While this nearly doubles the cost of the treatment, some choose to go this route in the hope of experiencing pregnancy together.
Key Questions About Reciprocal IVF
Whose Eggs? Whose womb?
This decision of whose eggs to use and who carries can be 100% personal, or there could be a significant advantage (from a success rate standpoint) or having a specific partner be the donor, and the other be the carrier. While there could be medical advantages for one partner to take a certain role, there can similarly be emotional, (psycho/physio)logical, and identity reasons for why one partner may be better suited to carry. For example, a trans man may be able to carry a pregnancy biologically, but may not to because it doesn’t align with their identity or because they’d have to cease testosterone treatment.
Regardless, it’s important to have both partners receive a full female fertility workup prior to starting a reciprocal IVF cycle as it can help identify who would be the best partner (or, in some cases, the only partner medically advised to act in a certain role).
As a general rule:
Whose eggs: The partner who is younger or that has a better ovarian reserve with no known genetic abnormalities.
Whose Womb: The partner who has the “healthier” uterus or who has had kids before and is healthy for pregnancy.
Of course, both partners could be relatively equal on these parameters making that decision primarily a personal one. There’s certainly no hard and set rule that comes here and is truly a personal decision that is usually best made by a couple after their fertility testing in the consultation with their doctor
Genetic Testing & Gender (sex) selection?
Genetic testing can be helpful for some, but many doctors question its importance, particularly for younger females who are at relatively low risk for having aneuploidy embryos. Aneuploidy embryos are those with an abnormal number of chromosomes that are at higher risk for miscarriage or failed implantation.
Besides older females that are at higher risk for aneuploidy, there are two other populations that can in general benefit greatly from genetic testing:
- Those looking to choose the sex of their child: Amazingly, genetic testing lets you choose the biological sex of a child with 100% accuracy with what is generally known as gender selection.
- Carriers or those affected by known genetic disorders: Genetic testing allows those who are at risk of passing on a genetic disorder to their child the ability to screen their embryos for genetic testing.
It’s important to remember that genetic testing increases the cost of reciprocal IVF on two folds. The cost of genetic testing itself can cost as much as $5,000 and also requires a frozen embryo transfer, which can similarly cost $5000 at some clinics. Of course, there is an incredible variation in cost for these services from clinic to clinic, so it’s important to get costs from your specific center.
1 or 2 embryos?
Transferring one or two embryos is one of the leading “controversies” of today’s fertility medicine. There was a time in its infancy where reproductive endocrinologists and other fertility specialists would routinely transfer multiple embryos. This practice was largely due to the uncertainty of individual embryo health and their ability to implant. By transferring multiple embryos, clinics were able to “improve,” their success rates, and boast superiority over other clinics. This outdated practice has developed some unwarranted “fear,” as people often think that if they do IVF that they will automatically have twins or, in rare cases, even higher number of multiples.
Today, most transfers are single embryo transfers as they result in the same success rates (when including FETs from that cycle) while essentially eliminating the risks associated with multiples pregnancy. While there are certain guidelines and restrictions that may require you to do a single embryo transfer, many clinics will, with the guidance and consultation of a doctor, transfer more than one embryo under certain circumstances.
Reciprocal IVF Success Rates
The success rates of reciprocal IVF, similar to the success rates of IVF vary greatly depending on the age of the “egg donor,” as well as any significant infertility diagnosis like endometriosis. Generally, the younger the donor, the higher the success rates. Given that those pursuing reciprocal IVF may be younger than the average couple undergoing IVF and are less likely to have significant infertility issues, it’s possible that the overall success rate is higher for those undergoing reciprocal IVF than those encountered by the general population.
As discussed earlier, IVF isn’t always successful on the first attempt. It’s important to understand that many will need multiple cycles to achieve a live birth. The chart analyses average success rates data through 6 cycles using a statistical analysis of successful outcomes given multiple trials of independent events. Because there is some evidence to suggest that the results of two IVF cycles are not truly independent (with slightly higher odds of a subsequently failed cycle if given a previously failed cycle), we subtracted a 3% from every successive cycle to provide a more realistic look across multiple cycles.
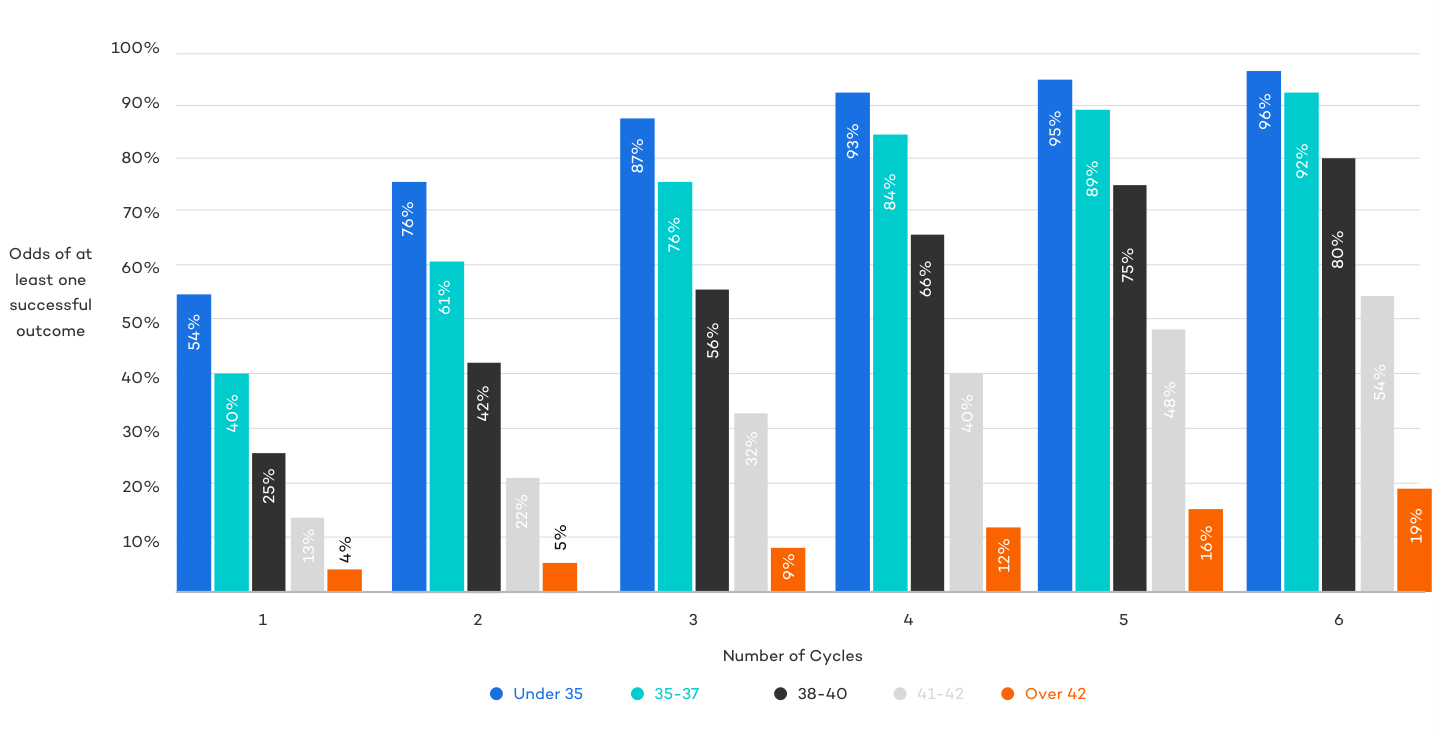
The Bottom Line
Reciprocal IVF is a fantastic treatment option for many in the LGBTQ community offering high success rates and an important bond with the child for both parents. Costs may be of concern for some, but given affordable options exist and the ability to finance much of the treatment, it can be pursued by many who may not have thought it was possible.