IVF Egg Retrieval: Process, Procedure, Recovery, Risks, and More
Egg retrieval is a key step in the IVF and egg freezing process. It entails mature eggs being collected from the ovaries through a short, minimally invasive procedure.
Though this may sound intimidating, the process is safe, typically painless with anesthesia, and recovery is usually quick. This step opens the door to either freezing eggs for future use or fertilizing them immediately to create embryos.
In this article, we’ll explore the ins and outs of IVF egg retrieval, so you are better informed and prepared to take this essential step towards reproductive empowerment.
Fast Facts About the IVF Egg Retrieval Procedure
What it is:
- A procedure to remove eggs from the ovaries for Egg Freezing or In Vitro Fertilization (IVF). It is minimally invasive, usually leaving no scars or stitches and requiring only a short recovery time.
Timing:
- Performed about 10–12 days after beginning hormone stimulation medications that help the ovaries produce multiple eggs.
Procedure length:
- Typically lasts 10–15 minutes from anesthesia administration to completion.
Recovery:
- Minimal recovery due to monitored anesthesia care (MAC) and the minimally invasive nature of the procedure. This is a same-day procedure that is often compared to a blood draw through the vaginal wall.
Risks:
- Generally low, but may include: Minor bleeding, Infection, and rare injury to the bowel or bladder. Your provider will review all risks with you and answer any questions you may have at the time of procedure consent.
What happens to the eggs:
- After retrieval, eggs are taken to an embryology lab where they may be:
- Frozen for future use
- Fertilized and cultured for 3–7 days
- Placed in an INVOcell device (less common) for fertilization and development
Next step in IVF:
- For patients proceeding with IVF, the following step is embryo transfer, when embryos are placed into the uterus of the intended parent or gestational carrier.
Egg Retrieval Process & Timelines

The egg extraction procedure begins with ovarian stimulation medications for IVF or egg freezing.
These medications usually start on days 2–4 of a woman’s natural menstrual cycle and continue for about nine to twelve days. For women without regular cycles, treatment can often begin at any time after a baseline evaluation of hormones, follicles, and uterine lining.
The length of stimulation depends on follicle growth. At each monitoring visit, ultrasound and bloodwork measure follicle size, hormone levels, and endometrial thickness. This information guides the timing of the retrieval.
Egg retrieval is always scheduled 35-36 hours after the trigger shot (Lupron or hCG). This medication prompts final egg maturation and prepares the body for ovulation.
Retrieval must happen before the follicles rupture and release the eggs. By timing it carefully, providers collect the eggs at their most mature stage, while still inside the follicles. Taking the trigger shot at the exact prescribed time is essential for success.
The exact “trigger day” can shift based on follicle development. If follicles are not yet ready, stimulation medications such as FSH and an antagonist (Cetrotide, Ganirelix) are continued until they reach the right size. Because timing and medication dosages can change, it helps to stay flexible and trust the process during IVF stimulation.
The Egg Extraction Procedure
Preparing for the procedure:
Most of the “do’s” and “don’ts” that will help improve the number and quality of eggs retrieved need to happen 30-90+ days prior to your retrieval.
So, while the night before is certainly important, it’s really what you do three months prior that has the most impact on your success. A healthy body is a fertile body: acupuncture, a high-fat fertility diet, overall healthy lifestyle choices, and supplemental vitamins are important.
The day of, relax, stay positive, and give yourself enough time to get to your provider’s office ahead of time without needing to rush.
That said, the egg retrieval is a procedure done under IV sedation, and it’s important you follow the instructions given by your healthcare team carefully. You’ll be asked to follow a number of instructions or precautions in preparation for your egg retrieval procedure.
Some common to-dos include:
- wearing comfortable, easy to remove clothing
- arriving early, usually an hour before the intended retrieval
- making sure you have a ride home. It’s usually recommended that a family member or a close friend accompany you to your egg retrieval, but other ride arrangements can be made if necessary. You won’t be allowed to drive for 24 hours after receiving the IV sedation.
Some important do-nots include:
- eating or drinking anything after midnight on the day of your procedure.
- wearing perfumes or fragrances other than deodorant the day of the egg retrieval procedure.
After you check in, you’ll likely change into a robe or hospital gown and be taken to one of the surgical suites. Once in the surgical suite, you’ll have blood drawn, complete some paperwork, consult with the nurse, anesthesiologist, and/or CRNA, provider performing the procedure, and a member of the embryology team.
The nurse will then hook you up to several monitors so that your vital signs can be closely monitored before, during, and after the procedure.
The Procedure
The Egg retrieval procedure begins with the anesthesiologist and/or CRNA administering light intravenous sedation for your comfort.
The anesthesiologist (or CRNA) will use MAC (monitored anesthesia care) as opposed to general anesthesia. While general anesthesia requires you to be intubated with an endotracheal tube so you can breathe during surgery, MAC offers deep sedation with no tube and a much faster recovery time.
Once you are sedated, your provider will then use a transvaginal ultrasound to locate the ovarian follicles. It is also a possibility to retrieve eggs through the abdomen if needed.
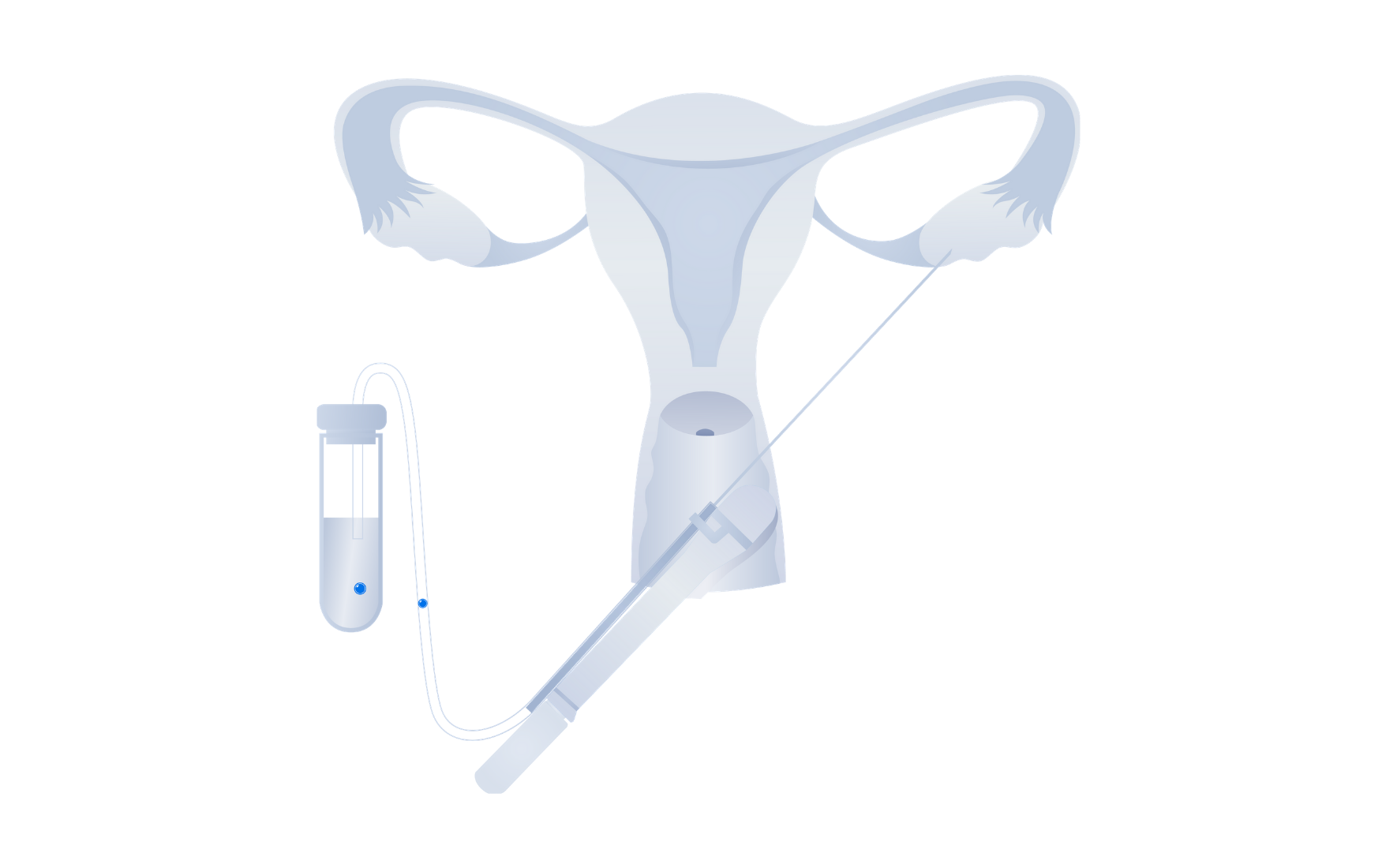
Then, using a tiny hollow needle with suction capabilities, your provider will guide the needle attached to a catheter through the vaginal wall and drain the fluid from the follicles, which contain the eggs.
The follicular fluid containing the eggs is drawn using light suction and collected in test tubes labeled with your name and patient ID.
Once collected, eggs are immediately transported to the embryology lab, where one of the embryologists will locate, isolate, and place your eggs in media where they will continue to develop for a few hours prior to freezing or fertilization.
The actual time it takes to locate and retrieve eggs is only about 5-15 minutes. There are no incisions or stitches. During the egg retrieval, anesthesia ensures you won’t feel pain or remember the procedure.
Once the retrieval is complete, the anesthesiologist (or CRNA) will gently bring you out of sedation, and you will be transferred to a recovery room where you’ll continue to be monitored.
It usually takes 5-10 minutes to return from sedation, and about 30 minutes to recover to normal consciousness, after which point, you are free to go home.
Before you go, one of the clinical team members will tell you how many eggs were retrieved. If you have additional questions or require additional pain medication, you will be taken care of before being discharged.
Egg Retrieval Recovery
We encourage those having an egg retrieval to take it easy on the day of the procedure. Rest and relax at home and catch up on your favorite series or watch a movie.
You’re clear to return to work the following day, barring any complications.
You can expect some discomfort after egg retrieval, such as:
- bloating
- mild vaginal soreness
- abdominal cramping
- light spotting.
These symptoms usually last a couple of days, and most people feel back to normal by the next day and/or their next menstrual period. Over-the-counter pain relievers like Tylenol or ibuprofen are often enough to help.
A follow-up appointment is rarely needed, but your care team is available if you have concerns. Call them right away if you experience excessive bloating, vomiting, severe pain, excessive bleeding, shortness of breath, or if you simply feel unwell. These may be signs of ovarian hyperstimulation syndrome (OHSS), a condition where the ovaries swell beyond what is normal and become painful after fertility medications.
Mild OHSS may cause abdominal pain, nausea, vomiting, diarrhea, or tenderness near the ovaries.
It often improves within several days to a week. Supportive care, such as a diet high in nutrient-dense, fatty, whole foods, and acupuncture, can help.
In more severe cases, medical attention may be required. OHSS usually develops within a week of the trigger shot, which is why close monitoring during your cycle is so important. If your provider sees signs of higher risk, they may adjust your medication or recommend freezing embryos for transfer at a later time, once your body has recovered.
To reduce constipation during recovery, stay well hydrated and consider using a stool softener if needed.
What Happens to the Eggs After Retrieval?
Immediately after retrieval, your eggs are transported to the embryology lab by the embryologists attending your egg retrieval.
The embryology team will then locate, count, and place your eggs in nourishing media that mimics the environment of your fallopian tubes. The eggs are then placed in an incubator labeled with your full name and medical record number.
At this point, if you’re freezing eggs, they can be flash-frozen via vitrification. Once cooled, the eggs are kept in liquid nitrogen cryotanks for preservation.
If you are freezing embryos or planning an IVF embryo transfer, the eggs will be fertilized approximately 4 hours after the retrieval and placed back in the incubator.
After this, the eggs are checked regularly for several days for fertilization and until the embryos reach a cleavage or blastocyst stage, at which point they will be frozen or transferred back into the carrier’s uterus.
IVF Embryo Development Timeline
- Day 0 – Egg Retrieval & Sperm Injection (ICSI or Conventional IVF)
Eggs are retrieved and fertilized, either through conventional IVF or intracytoplasmic sperm injection (ICSI). - Day 1 – Fertilization Check
About 14–16 hours after ICSI, an embryologist examines the eggs to confirm fertilization. - Day 2 – Early Cell Division
Embryos begin to divide. Most labs do not check embryos on this day. - Day 3 – Cleavage Stage, Grading, and Possible Transfer
Embryos are graded based on cell number and quality. A healthy Day 3 embryo usually has 6–10 cells. Research shows embryos in this range are more likely to progress to the blastocyst stage. Grading also assesses cell uniformity and fragmentation. A Grade 1 embryo has evenly sized cells with no visible fragmentation. - Day 4 – Transition to Blastocyst
Embryos shift from the cleavage stage to the blastocyst stage. Most labs do not check embryos on this day. - Day 5 – Blastocyst Stage, Grading, Transfer, or Freezing
Embryos are evaluated again. Those that reach blastocyst stage may be transferred into the uterus or frozen for future use. - Days 6 & 7 – Extended Blastocyst Development
Embryos that do not reach blastocyst stage by Day 5 are re-checked. Those that progress can be transferred or frozen. Embryos that fail to develop into blastocysts are not considered viable and are typically discarded.
What are the next steps after egg retrieval?
The next steps after egg retrieval depend on whether you are
- doing egg freezing or IVF
- planning a fresh or frozen transfer
If you’re egg freezing, the process is complete until you decide later to thaw, fertilize, and transfer the embryos made from your frozen eggs.
If you are planning on doing an embryo transfer, the decision to take your embryos to the cleavage or blastocyst stage is usually made after seeing the number of fertilized embryos.
Suppose there are four or more fertilized eggs (now embryos), we usually recommend taking the embryos to the blastocyst stage.
If there are fewer embryos, we usually recommend preparing for a day three transfer or a day 3 freeze. You will typically be contacted the day after retrieval and informed of how many were fertilized.
If planning on taking your embryos to blastocyst, you will not be contacted until day 7 or 8. If planning on taking the embryos to the cleavage stage, you should be contacted on day three.
If you’re planning to have a fresh embryo transfer, you will likely start taking estrogen and progesterone the day after your retrieval to help prepare the lining of your uterus for implantation.
If planning a frozen embryo transfer, you will likely rest until the start of your next cycle, in which you will take estrogen and progesterone to prepare the uterus for implantation.
Average Number of Eggs Retrieved by Age
So, how many eggs should you expect to retrieve? It will vary from person to person and cycle to cycle for the same person. But experts generally regard 10-15 mature eggs as being an optimal number of eggs.
Researchers in a analyzed more than 400,000 IVF cycles in the United Kingdom. They found there was a strong association between the number of eggs retrieved in one IVF cycle and live birth rates. The likelihood of success rose with each additional egg retrieved, up to about 15 eggs. Outcomes leveled off when 15-20 eggs were retrieved, and then steadily declined beyond 20 eggs.
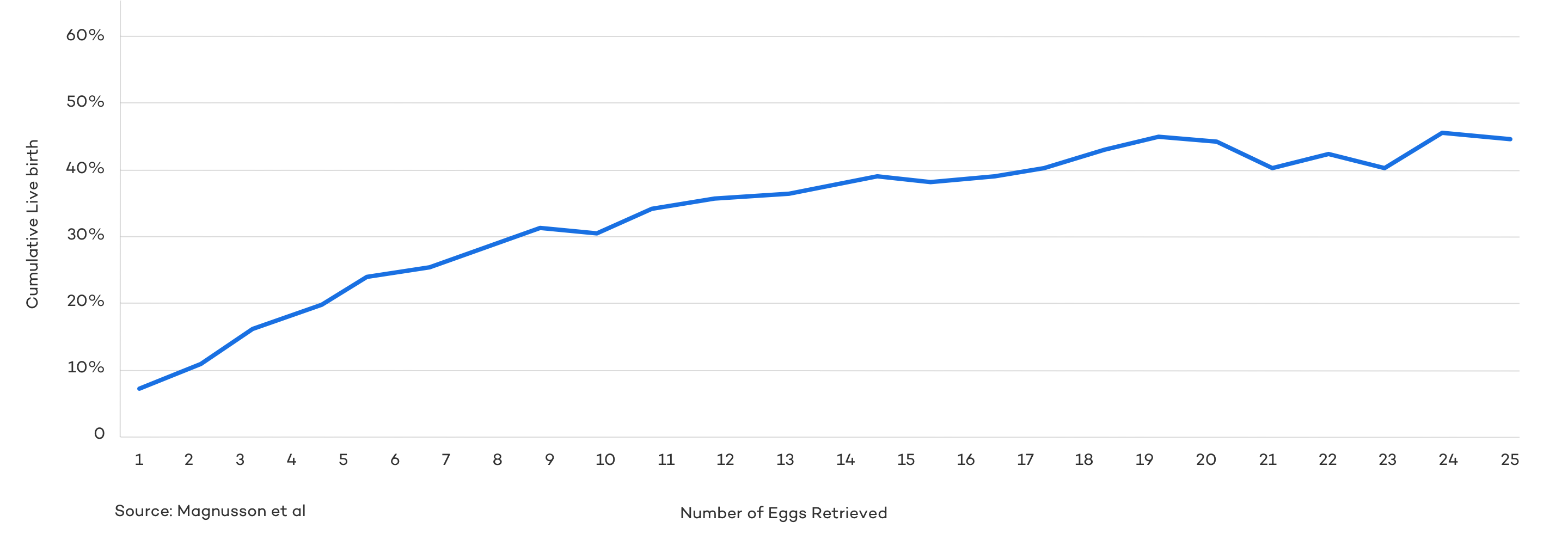
Quality is always more important than quantity, and IVF success requires only one normal embryo, but patient outcomes improve when a reasonable number of eggs are retrieved, typically between 10-15 mature eggs.
Younger women under the age of 35 tend to produce more eggs than older women. Women who respond better to ovarian stimulation will produce more eggs than women who are low responders. Women who produce 20 or more eggs are usually young females with no fertility problems.
Egg Retrieval Risks & Side Effects
No two women are alike, so each may experience different post-retrieval symptoms. The major side effects of egg retrieval can include constipation, bloating and cramping, breast tenderness, discharge, infection, and OHSS. Risks associated with anesthesia are usually very minimal.
- Constipation: One of the most common side effects women report after egg retrieval surgery is constipation. Take a stool softener if necessary, and be sure to stay hydrated.
- Bloating & Cramping: Because your ovaries become enlarged after IVF stimulation and egg retrieval, it’s not uncommon to feel mild to moderate cramping after you return home. Hormones can create bloating, too. Increasing consumption of protein can be very helpful.
- Breast Tenderness: Rapidly changing hormone levels can create sore or tender breasts, similar to what some women experience during premenstrual syndrome (PMS). After your procedure, be sure to wear a supportive bra to avoid putting any unnecessary strain on your chest and take OTC pain medication if necessary.
- Vaginal Discharge: It’s not uncommon to pass small amounts of watery fluid. Because the cervix is cleaned before egg retrieval, some discharge can get left behind, which is later passed. While it’s often clear, patients may experience bloody discharge as well. It’s important not to strain while following the procedure, either while using the toilet or through heavy lifting or activity. Excessive straining can further irritate the cervix.
- Infection: During any surgical procedure, infection is always a risk. The use of an aspirating needle to collect eggs can potentially cause bleeding, infection, or damage to the bowel, bladder, or a blood vessel.
- Ovarian Hyperstimulation Syndrome: symptoms can range from mild to moderate abdominal pain, abdominal bloating, nausea, vomiting, diarrhea, and tenderness near the ovaries, to severe symptoms like rapid weight gain (more than 2.2 pounds in 24 hours), severe abdominal pain, persistent and severe nausea and vomiting, blood clots, decreased urination, shortness of breath, and a tight or enlarged abdomen. Severe symptoms should be addressed with your provider as soon as possible and may require treatment. As mentioned previously, acupuncture and increased protein consumption can greatly reduce the symptoms of OHSS.
How to Improve Egg Retrieval Outcomes
Egg development takes 90 days; use it wisely.
IVF only targets the final developmental phase of egg production taking place in the last 10-14 days. To improve egg retrieval outcomes, women need to be sure they’re doing everything possible to improve the quality of their eggs for the full 90 days prior to retrieval. Egg quality is a major factor impacting IVF success, and something you have the power to influence.
At CNY Fertility, we recommend women eat a high fat, moderate protein, low carbohydrate (AKA ketogenic) diet, take high-quality supplements that can improve egg quality, and prescription medications (if necessary) to reduce inflammation, improve implantation, and regulate the immune system.
A of the effects of coenzyme Q10 found it boosted ovarian response in younger women with low ovarian reserve. Similarly, acupuncture can be helpful.
Consider Additional Surgical Interventions and Therapies:
If you’ve had recurrent pregnancy loss or recurrent implantation failure (specifically three failed euploid embryo transfers), consider a laparoscopy and hysteroscopy.
There are also various procedures, such as PRP-Therapy, along with yoga, massage, and acupuncture, that CNY Fertility providers recommend as part of a protocol to boost female fertility.
Be Proactive if you have PCOS:
Patients with PCOS are at higher risk for developing OHSS. An alternate trigger shot is frequently chosen for these patients, and freezing embryos for a frozen embryo transfer (FET) is recommended to give the body time to recover. It’s critical that patients with PCOS begin preparing for egg retrieval from 90 days up to 6-months in advance, to reduce BMI and inflammation, possible insulin resistance, and maximize health so that retrieval can be successful and safe.
A high-fat, moderate-protein, low-carb diet is critical for getting pregnant with PCOS.
Follow Trigger Instructions to a ‘T’:
Egg retrievals happen in the morning, so you’ll be administering your trigger shot two evenings earlier. Inject at exactly the time you’ve been instructed. If you’re traveling for treatment, check the time difference. Be sure to store your injectables correctly. Remember to set an alarm!
Talk to Friends & Family and be sure you have the support you need:
The time before, during, and immediately after an IVF cycle can be very stressful. Ensure you are reaching out for the support you need.
Support groups are a tremendous resource for emotional support. Mentors who have been in your shoes offer a caring ear and great advice for managing any stressors and emotions. If you’re more comfortable one-on-one, go that route. Just be sure you reach out and don’t suppress your stress.
The Bottom Line
The egg retrieval procedure is one of the most important steps in the IVF Process. It, along with the steps leading up to and coming after the egg retrieval make IVF the most effective fertility treatment as it works its way around a number of key fertility issues.
The egg retrieval is a relatively simple procedure with little risks. During the egg retrieval, a fertility provider uses a hollow needle to drain the follicles of their fluid (an egg retrieval can easily be thought of like a blood draw through the vaginal wall) which contains the woman’s eggs. After the egg retrieval, the woman usually prepares for an embryo transfer or her eggs are frozen for future use..



