Recurrent Pregnancy Loss

The odds of experiencing a miscarriage vary greatly by age, but on the whole, approximately 20-25% of pregnancies end in loss. Most pregnancy losses are due to random genetic mutations in the developing embryo and many take place before a pregnancy is even identified by the mother. While any loss is incredibly tragic, the random nature of most pregnancy losses means that there usually isn’t much concern medically speaking. That is until a woman experiences recurrent pregnancy loss.
Recurrent pregnancy loss, as defined by the American College of Obstetrics and Gynecology (ACOG), is experiencing two or more miscarriages. That said, a thorough exam and workup usually aren’t performed until after a woman’s third pregnancy loss.
As women get older, the amount of genetically abnormal eggs and resulting embryos they produce increases. These mutations are random, but they make older women more likely to experience pregnancy loss.
Several other factors like systematic inflammation, autoimmunity, and more are also associated with an increased risk of miscarriage and likely have a significant impact on those experiencing recurrent pregnancy loss.
Fortunately, new advancements have been made in the field of reproductive immunology which can help patients gain clarity and treat their recurrent miscarriages and IVF implantation failures.
This article will cover the most common causes of recurrent pregnancy loss along with testing and treatment options for recurrent miscarriages.
Fast Facts about Recurrent Miscarriage
- Up to 26% of all pregnancies end in miscarriage.
- Recurrent pregnancy loss, as defined by the American College of Obstetrics and Gynecology (ACOG), is experiencing two or more miscarriages.
- Approximately 1% of women will experience recurrent pregnancy loss and have repeated miscarriages.
- The most common cause of pregnancy loss occurs when embryos contain chromosomal abnormalities. Women of any age produce abnormal eggs, but as women get older, the proportion of chromosomally abnormal eggs they produce and resulting embryos increases. Therefore, in addition to an increased possibility of miscarriage, their chances of getting pregnant also decrease. PGT-A Embryonic Genetic Testing can be used to screen for genetically abnormal embryos.
- For up to 50% of patients who experience recurrent pregnancy loss, there is no clearly defined cause.
- Many cases of recurrent pregnancy loss are caused by Parental Compatibility (HLA mismatches), Natural Killer Cell, Cytotoxic Activity, Systemic Inflammation, Thrombophilia, Regulatory T-cell, and Autoimmunity. These issues are not easily identified but can be screened for using state-of-the-art immunological testing developed by Pregmune.
- Reproductive immunology treatment should be considered for patients who experience two failed IVF transfers or miscarriages.
- Genetically testing embryos and performing immunological testing can help to significantly reduce the chance of miscarriage and increase the odds of a live birth.
What Are The Most Common Causes of Recurrent Pregnancy Loss?
The most common cause of recurrent miscarriages is chromosomal abnormalities.
However, several other factors which are historically less understood, mainly immunological reasons and inflammation, can also cause recurrent pregnancy loss and play a significant factor in occurrences of recurrent miscarriage, particularly those labeled as “unexplained.”
Uterine abnormalities and hormonal disorders are also linked to recurrent pregnancy loss.
Genetic Abnormalities
Genetic abnormalities can be caused by genetically abnormal eggs, sperm, or may originate in the embryo itself after fertilization or normal egg and sperm has taken place.
Chromosomally abnormalities occur in two forms; (1) numerical abnormalities (aneuploidy), such as a missing or an extra chromosome, or (2) structural abnormalities, where there is an issue with the structure of a chromosome.
As women get older, the amount of genetically abnormal eggs and embryos she produces increases.
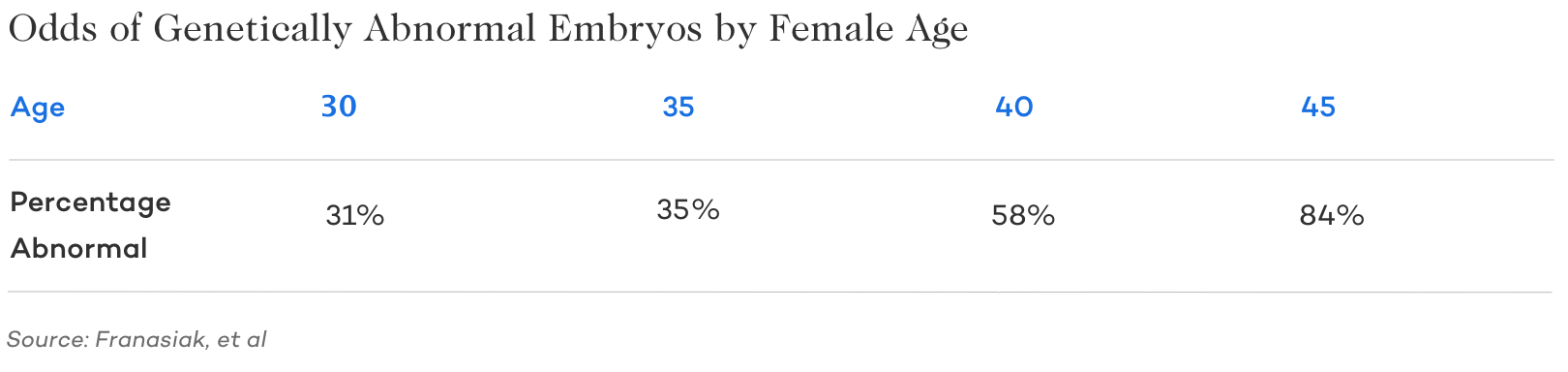
Due to the increased number of genetically abnormal embryos they produce, older women are at a greater risk of experiencing a miscarriage.
As mentioned above, genetically abnormal sperm is another cause of recurrent miscarriages. Sperm from couples with a history of recurrent pregnancy loss are more likely to be abnormal and have an increase of sex chromosome disomy (an extra chromosome). Similar to how women’s eggs decrease in quality with age, sperm DNA damage has been linked to increasing paternal age. However, the exact link(s) between increased paternal age and recurrent pregnancy loss have not been identified. Genetic abnormalities in sperm and the resulting affected embryos are considered “understudied.”
Immunological Reasons and Recurrent Pregnancy Loss
The implantation of a pregnancy is a complex immunological process. Since the fetus is not genetically identical to its mother, certain immunologic events can occur which cause the body to reject the fetus. Many different mechanisms have been proposed for why the mother’s body does not carry the fetus all the way throughout gestation.
As such, fertility specialists and researchers believe abnormalities within the mother’s immunologic mechanisms can cause recurrent miscarriages. These issues are not easily identified but can be screened for using state-of-the-art immunological testing through Pregmune. Many cases of recurrent pregnancy loss are caused by Parental Compatibility (HLA mismatches), Natural Killer Cell, Cytotoxic Activity, Systemic Inflammation, Thrombophilia, Regulatory T-cell, and Autoimmunity.
Fetal HLA-C and Maternal KIR (Uterine NK Cell) Interaction
Establishing pregnancy and embryo implantation are complex processes that are accompanied by maternal hormonal changes, immune responses, and embryo growth and maturation. For successful implantation to occur, these events must be synchronized. Some reproductive endocrinologists believe that uterine natural killer cells (NK) may impact these processes and result in reduced reproductive performance.
Increased numbers of uterine natural killer cells have been associated with reproductive failure. As such, some fertility specialists are diagnostically testing and checking the level of natural killer cells in a woman’s blood to guide treatment and therapy recommendations to reduce the chances of recurrent miscarriage and implantation failures.
Thrombophilia
Thrombophilia by definition is when your blood forms clots too easily. Thrombophilia increases the risk of deep vein thrombosis and is associated with recurrent pregnancy loss. Thrombophilia is linked to elevated homocysteine levels.
MTHFR (5, 10 methylenetetrahydrofolate reductase) is a protein that is crucial to maintain optimal levels of circulating folate and methionine and is key to prevent the accumulation of homocysteine. Homocysteine accumulation can lead to inflammation and pregnancy complications that contribute to recurrent miscarriages.
MTHFR levels can be tested through blood tests offered by Pregmune. The results of Pregmune testing help fertility specialists to assess the level of risk for thrombophilia which allows them to make appropriate treatment recommendations. In addition to MTFHR levels, Pregmune testing also checks if you carry a specific allele that may increase PAI-1 activity thus increasing your risk for blood clots and miscarriage.
Antiphospholipid Antibodies
Antiphospholipid autoantibodies syndrome (APS) is an autoantibody-mediated disorder where antiphospholipid antibodies are produced by the immune system against itself. This can lead to blood clots, multiple miscarriages, and other pregnancy complications.
There is growing evidence that supports that APS is a cause of recurrent spontaneous abortion. Research indicates that 7-25% of recurrent miscarriage cases have antiphospholipid antibodies as the main risk factor.
Pregmune testing aims to detect the presence of these antibodies in your blood.
Inflammation
Inflammation is another common cause of recurrent miscarriage. Research has shown that inflammation plays a vital role in both implantation and miscarriage. Inflammation is the immune system’s response to what it perceives as harmful stimuli. When a woman gets pregnant, since the fetus is not genetically identical to the mother, sometimes the body treats the fetus as an invader. During implantation, the immune system can cause an inflammatory response which contributes to pregnancy loss.
Additional research confirms that during pregnancy there is an inflammatory reaction that may be disrupted during a miscarriage.
Uterine Abnormalities and Recurrent Pregnancy Loss
Research shows that congenital and acquired uterine abnormalities are associated with recurrent pregnancy loss.
Uterine abnormalities or Müllerian duct anomalies are fairly uncommon (occurring in about 0.5% of women), but they can affect a woman’s fertility and cause recurrent miscarriages. Uterine abnormalities are either present from birth or are acquired over time. For a normal uterus, development begins with two tube-shaped structures known as the Müllerian ducts. These ducts come together to form the uterus. For women with Müllerian duct anomalies, the connection between these two ducts is incomplete.
Many women with uterine anomalies do not require treatment and are able to sustain pregnancy on their own. Other women who experience pain, infertility, or miscarriage do require surgery. Most anomalies can be corrected using minimally invasive techniques like surgical laparoscopy – hysteroscopy.
Hormonal Disorders – Diabetes, Polycystic Ovary Syndrom (PCOS), Thyroid Disease
Hormonal disorders like diabetes, Polycystic Ovary Syndrom (PCOS), and thyroid disease can also contribute to recurrent pregnancy loss. In fact, researchers estimate that endocrinal disorders may contribute to anywhere from 12-18% of recurrent pregnancy loss cases.
Proper hormone levels are needed for a successful pregnancy. Hormonal disorders can cause elevated levels of androgens, the hormone prolactin, or others which can interfere with pregnancy and cause miscarriage.
How is Recurrent Pregnancy Loss Evaluated – Recurrent Miscarriage Testing
Following a second miscarriage, it is recommended that you go for testing to detect what may have caused the previous miscarriages. Basic testing includes;
- blood tests
- ultrasound tests (usually a pelvic ultrasound)
- pelvic and uterine exams
- chromosome tests – karyotype analysis of both partners
After a miscarriage, blood tests are completed to check for hormonal imbalances, gene mutations, or underlying health conditions that may be contributing to recurrent miscarriages. Other tests may be recommended based on the patient’s history and age, like insulin testing, ovarian reserve testing, antibody testing, etc. Chromosomal testing can be completed by way of a blood test on the parents, including karyotype analysis and testing for single-gene disorders.
Ultrasounds are completed to get a clear image and check the status of the uterus. Pelvic and uterine exams are completed to check if the cervix is opening or if there is a blockage caused by tissue or blood buildup.
After the ultrasound, your doctor or fertility specialist may recommend a saline ultrasound, hysterosalpingogram (HSG), MRI, or a hysteroscopy to further assess the status of the uterus and check for abnormalities like polyps, fibroids, or scarring.
Testing can also be completed on the product of conception to check for chromosomal abnormalities.
Still, after all of the above standard testing is completed, recurrent pregnancy loss remains “unexplained” in 45-50% of patients.
Pregmune
CNY Fertility and some other fertility clinics now offer a new testing and reporting platform for the immunological evaluation of miscarriage and infertility that can help guide the immune treatment with even more precision.
The report was developed by a team of reproductive immunologists and is created by a medical company called PREGMUNE. The Pregmune PGM-1 Reproductive Immunology Assessment Report will help identify the potential causes of your infertility, estimate your chances for successful live birth based on their customized artificial intelligence algorithm, and will provide you with expert guidance for follow-up treatment for an improved chance of success.
Specific to recurrent pregnancy loss, Pregmune blood tests check for:
- uterine killer cells (NK cells)
- anti – HLA antibodies
- thrombophilia
- vitamin D levels
- folate levels
- and more
Treating Recurrent Pregnancy Loss
Treatment for recurrent miscarriage is based on the underlying cause of the condition. For example, if a uterine abnormality is discovered, then surgery may be indicated.
Based on the blood test results, medications may be recommended to treat any underlying conditions that are discovered. For example, if diabetes or thyroid dysfunction is discovered then medications can be prescribed.
If it is discovered that one or both of the parents have chromosomal or genetic abnormalities, then IVF with genetic testing is recommended.
Genetic Testing to Reduce Miscarriage Rates
Pre-Implantation Genetic Testing (PGT) can be completed to test embryos for chromosomal abnormalities during the IVF process after they are retrieved and before they are transferred back to the uterus. Genetic testing is most commonly recommended for women over the age of 35 as the number of genetically abnormal embryos women produce increases with age.
Research has shown that abnormal embryos can significantly increase the chance of miscarriage.
The figure below displays data provided by Cooper Genomics on how Pre-implementation Genetic Testing for Aneuploidy (PGT-A) testing can decrease the rate of miscarriage across several different age groups – particularly notable is the data as one gets closer to and beyond 40.
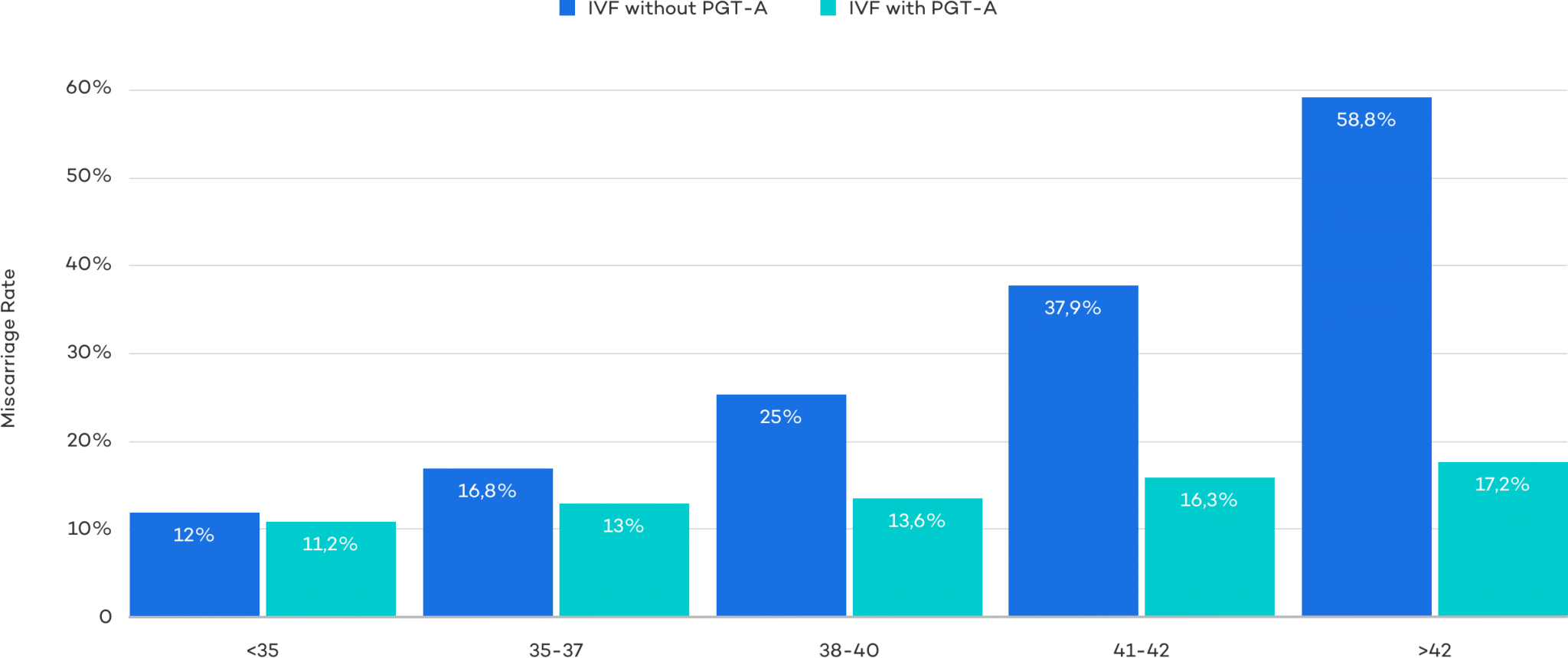
PGT-A is just one form of genetic testing and it can be a valuable tool for couples who are experiencing recurrent pregnancy loss.
As mentioned above, approximately 50% of patients who experience recurrent pregnancy loss receive a diagnosis of “unexplained.” If traditional recurrent pregnancy loss testing doesn’t produce a clear result, then there are other options.
Intralipids
Intralipids are essentially IV-administered fats. They are synthetic and made from 1.2% egg yolk phospholipids, 10% soybean oil, 2.25% glycerin, and water. Intralipids are administered 4-7 days prior to embryo transfer or insemination to improve implantation and reduce pregnancy loss by lowering the activity of the natural killer cells in our immune system.
As the result of a clinical trial, researchers concluded that intralipid infusion can improve the outcome in natural killer cell positive females with a history of recurrent miscarriages undergoing IVF/ICSI cycles.
Low Dose Naltrexone (LDN)
LDN was developed to block the effects of opioid medications and treat addiction. LDN is just one of several protocols used at CNY Fertility to enhance oocyte implantation. LDN acts as an immunomodulatory (immune system modulator) and increases the body’s ability to heal itself. For fertility, LDN treatment is started on the first day of stimulation medications and is often continued throughout pregnancy. LDN treatment is temporarily stopped 4 days before oocyte retrieval and resumed the following day.
LDN causes the immune system to function at optimal levels which helps to correct hormonal imbalances in the body which cause problems for women with PCOS and who experience infertility.
Antibiotics
Antibiotics are medications that work by slowing down or stopping the growth of bacteria. Antibiotic therapy with IVF treatment can be used to eradicate bacteria and toxic byproducts which cause inflammation within the reproductive system. As mentioned above, inflammation can cause implantation failures and miscarriage.
Antibiotics can be used during IVF treatment to reduce the risk of infection for both men and women.
Prograf
Prograf is an immunosuppressant that was originally created as an anti-rejection medication for organ transplant recipients. As mentioned above, since the fetus is not genetically identical to the mother, certain immunologic events can occur which cause the body to reject the fetus.
Because the immune system is believed to play a role in infertility, Prograf is prescribed to women with a history of recurrent pregnancy loss or implantation failure.
Prednisone
Prednisolone is a synthetic hormone that helps suppress immune responses like inflammation. Its anti-inflammatory and immuno-suppressive abilities can treat a range of conditions and fertility issues.
Prednisone is prescribed to women with recurrent miscarriages, especially those with elevated natural killer (NK) cells. Prednisolone is prescribed for short-term use during the stimulation phase of fertility treatment to patients with elevated NK levels, a history of implantation failure, and recurrent miscarriages.
Low-Dose Aspirin
Aspirin is a non-steroidal anti-inflammatory medication and blood thinner. Research indicates that low-dose Aspiring (81) mg may improve pregnancy chances for women with a history of recurrent miscarriages. Aspirin can help reduce the risk of miscarriage, particularly in women with blood disorders, and lower the risk of developing pre-eclampsia and high blood pressure during pregnancy.
Low-dose aspirin treatment has been shown to increase pregnancy rates for patients undergoing IVF treatment by improving ovarian responsiveness, uterine and ovarian blood flow velocity, and implantation.
Lovenox (Enoxaparin)
Lovenox is an anticoagulant injection that is primarily used to treat and prevent deep vein thrombosis and pulmonary embolism during pregnancy and following certain types of surgery.
Since Lovenox helps prevent blood clotting, it can be used for those undergoing fertility treatment and it is usually started several days before embryo transfer. Lovenox can also be prescribed in cases of recurrent miscarriage, especially when there’s a known blood-clotting disorder. Lovenox can also be used to prevent blood from thickening – a side effect of high dosage estrogen treatment that is common in fertility treatments.
HCG Wash
During a normal pregnancy, HCG production is triggered by the embryo growing in the fallopian tube. In an IVF cycle, HCG is absent in the uterus because the embryos are in a dish, not in the fallopian tube. An HCG wash places HCG into the endometrium prior to the embryo transfer to create a “sticky” uterus and to improve the chances of successful implantation.
There is evidence that shows that placing HCG into the endometrium improves the response of the endometrium to the embryo so it is “ready” at the time of transfer. This is a uterine infusion.
Intravenous Immune Globulin (IVIG)
IVIG is made up of human antibodies. These antibodies are proteins naturally produced by the body to fight infections. I VIG therapy is recommended for fertility patients who have recurrent implantation failure or recurrent pregnancy loss. It is especially recommended to increase the chances of conception and carrying a pregnancy to term for women who have tested positive for natural killer cells and have experienced multiple miscarriages or implantation failures.
Fertility specialists aren’t exactly sure how IVIG works, but studies suggest that it may reduce the number of natural killer (NK) cells in the body. IVIG may also work by absorbing or blocking a woman’s antibodies, which can cause the body to attack the pregnancy as a foreign invader.
During a treatment session, IVIG is introduced to the body very slowly through an intravenous drip in the arm, possibly taking several hours. It is recommended that IVIG be administered prior to embryo transfer, and then two additional times following a positive pregnancy test.
Filgrastim (Neupogen)
Neupogen is a medication the number of white blood cells in the body. The increased amount of white blood cells suppresses the immune system and keeps it from attacking the embryo. For women with autoimmune disorder or PCOS, it can temporarily shut down the immune systems.
Neupogen is administered either in injection form or as a uterine wash. Neupogen is increasingly utilized for other conditions including the treatment of recurrent miscarriage and/or implantation failure. Neupogen is not yet approved or disapproved by the Federal Drug Administration (FDA) for these conditions or diagnoses.
Sildenafil (Viagra)
Research shows that Viagara therapy can help significantly decrease NK cell activity and increase endometrial thickness. Viagra works as a vasodilator that improves blood flow and nutrition delivery to the uterus. It is administered to women as a vaginal suppository.
The endometrial lining, also known as the uterine lining, normally thickens on its own in preparation of an embryo, but not always. The improved blood flow from Viagara treatment can help to improve the condition and thickness of the endometrial lining.
Embryo thickness is a significant factor in embryo implantation during IVF.
Metformin
Metformin for PCOS is primarily used to help regulate and lower insulin levels, balance the metabolic system, increase ovulation and reduce excess androgen production. Specific to recurrent miscarriages, metformin has also been shown to significantly reduce the rate of early pregnancy loss in women with PCOS.
Folate Supplementation
Fertility supplements play an important role in preconception and prenatal health, perhaps none more famously than Folate before and during pregnancy. Folate is extremely important for maternal health during pregnancy as it has been shown to reduce the risk of pregnancy-related complications, including preeclampsia and preterm birth.
It is recommended that women planning to get pregnant, even if they are not struggling with infertility, start taking folate at least one month before conception and continue taking folate throughout pregnancy.
Pregmune testing assesses the level of folate in a woman’s blood to reduce the risk of recurrent pregnancy loss.
+ We recommend supplementing with Molecular Fertility’s Peak Prenatal.
Omega 3 Supplementation
Omega 3s are known to have a laundry list of benefits for those trying to get pregnant and those who already are pregnant. Omega 3s provide women’s bodies with wonderful anti-inflammatory support.
Heightened levels of omega 3s during pregnancy are also associated with all of the following; brain and eye development, higher intelligence, better communication, and social skills, fewer behavioral problems, decreased risk of developmental delay decreased risk of ADHD, autism, and cerebral palsy.
For women with a history of recurrent miscarriage, omega 3s have been used in combination with low-dose aspirin to improve uterine artery blood flow.
+ We recommend the ultra-potent VivoMega Fish Oil that offers 6-8x the omega 3s per serving as your standard over the counter fish oil.
Vitamin D Supplementation
Vitamin D deficiency has been linked with recurrent pregnancy loss. The effects of vitamin D deficiency during pregnancy are well documented and they include all of the following; preeclampsia, gestational diabetes, fetal growth restriction, preterm labor, and spontaneous abortion. Researchers speculate that vitamin D supplementation can be used as a treatment in recurrent pregnancy loss patients.
Sample Protocols for Treating Recurrent Miscarriage
At CNY Fertility, we use 4 main stages in our reproductive immunology-based enhancement protocols. Of course, there are still things you can add on and mix out… but the below is a good representation of how we use the above-mentioned medications. Protocol one is often used to improve the success of first-time IVF cycles.
Pay special attention to protocols two, three, and four as they are typically used after failed IVF cycles, recurrent pregnancy loss, or to treat other known immunological dysfunction.
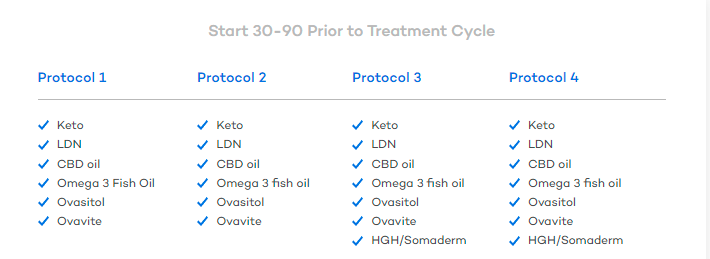
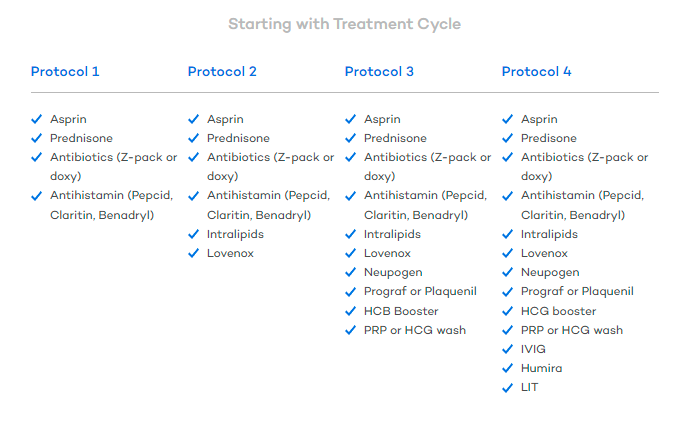
Check out our boost female fertility page for more dietary recommendations, medications, and immune and enhancement protocols, and other ways to reduce the risk of recurrent pregnancy loss.
Recurrent Miscarriage Coaching and Counseling
Pregnancy loss is shocking and traumatic for women and couples. Nearly 20% of women who experience a miscarriage become symptomatic for depression and/or anxiety. These feelings are very real and can impact your quality of life and future ability to achieve pregnancy.
Those who have experienced multiple losses are likely to feel even more shame or stress as a result of the repeated traumas. Shame can put stress on your relationship and stress is known to impact both male and female fertility significantly.
A history of miscarriage can bring about feelings of anxiety while trying to get pregnant, and once pregnancy is established again. As such, it is essential to take care of yourself and be mindful of your feelings.
So be kind to yourself and your partner if you are experiencing recurrent pregnancy loss. Consider speaking with a fertility specialist about your options, getting support from a mental health specialist, or exploring alternative options like fertility coaching. Here at CNY Fertility, we have developed a team of coaches and experts to help support people through life-changing moments at The Fertile Spirit.
In Conclusion
If you have experienced two or more miscarriages, it is recommended that you go for testing and seek the assistance of a fertility specialist specially trained in reproductive immunology. They can help to recommend appropriate treatment to reduce your chances of another pregnancy loss. At CNY Fertility, we employ state-of-the-art research on reproductive immunology and inflammation and technologies like genetic testing, Pregmune reproductive immunology assessments, and more to provide answers and help you on your fertility journey.
CNY Fertility’s founder and director, Dr. Kiltz, was one of the first reproductive specialists to study and apply the principles of reproductive immunology to infertility treatment and recurrent pregnancy loss. Because of this, people seek our CNY’s expertise from around the world in treating recurrent pregnancy loss which enables us to treat a large number of people needing reproductive immunology and develop an unmatched level of expertise.
Click here to schedule a consultation and speak with our team of fertility specialists!