Intracytoplasmic Sperm Injection (ICSI) in IVF: How the ICSI Procedure Works, Who It Helps, and What to Expect
Quick Answer: What is ICSI
Intracytoplasmic sperm injection (ICSI) is a laboratory technique used during in vitro fertilization (IVF) in which a single sperm is injected directly into a mature egg to achieve fertilization. The procedure is commonly used for male factor infertility or when fertilization may be difficult with conventional IVF.
Quick facts About ICSI IVF
Intracytoplasmic sperm injection (ICSI) is an advanced lab technique used during IVF to help with fertilization.
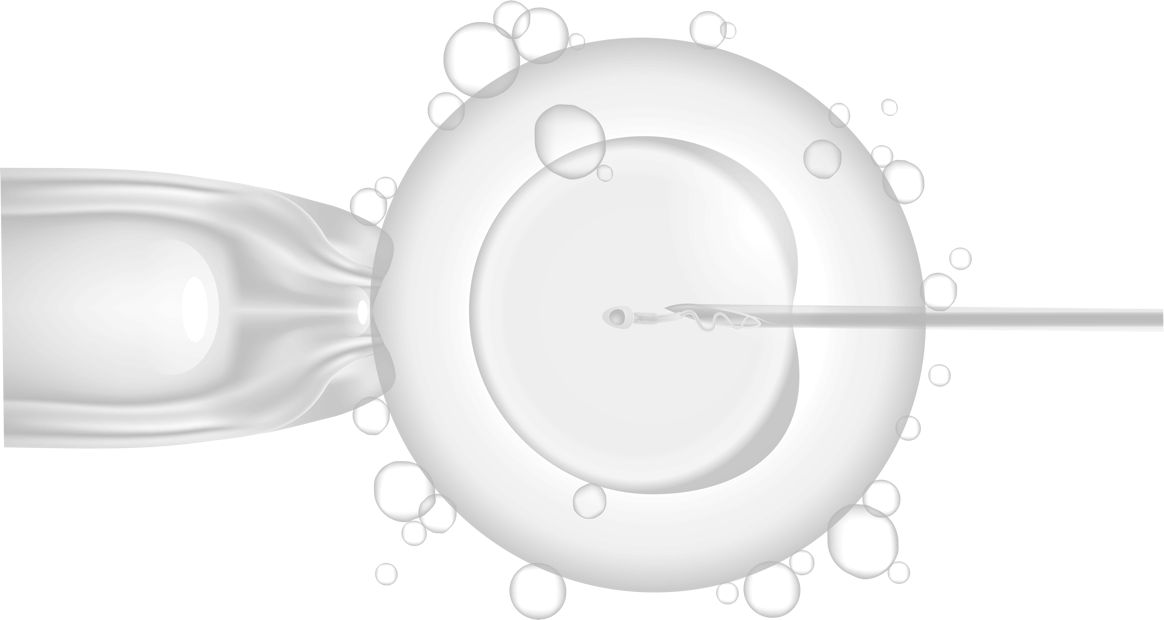
In ICSI, a single sperm is injected directly into a mature egg, bypassing the steps the sperm normally completes to penetrate and fertilize an egg on its own.
ICSI was originally developed to help overcome male factor infertility (such as very low sperm count or low motility), but over time, it has also become widely used in many IVF cycles, including some without clear male factor infertility.
What is ICSI in IVF?
ICSI is one of two main fertilization methods used in IVF:
- Conventional IVF insemination: many sperm are placed with each egg in a dish in hopes that fertilization happens “on its own” if the sperm successfully penetrates the egg.
A helpful way to think about it is that IVF bypasses the fallopian tubes, while ICSI bypasses several of the final sperm-to-egg steps that can fail in male factor infertility.
The ICSI procedure: step-by-step (what happens in the lab)
ICSI is performed by an embryologist using micromanipulation tools under a specialized microscope. While exact lab workflows vary, the core steps are consistent:
1. Egg assessment and preparation (denudation)
Eggs are surrounded by cumulus/granulosa cells. For ICSI, labs typically remove these cells so the embryologist can confirm egg maturity and safely perform injection.
2. Only mature eggs are injected
ICSI is typically performed only on fully mature eggs. In the lab, embryologists often look for a small “polar body” on the egg as a sign that the egg is ready for injection.
3. Sperm selection
The embryologist selects sperm with the best available movement and shape from the processed specimen (or surgically retrieved sperm, depending on the case).
4. Microinjection
Each egg is held steady with a holding pipette while a thin injection needle passes through the zona pellucida and deposits a single sperm into the egg cytoplasm. cytoplasm.
5. Fertilization check (the next morning)
Eggs are assessed for normal fertilization (typically, evidence of two pronuclei), and normally fertilized eggs are cultured into embryos for transfer or freezing.
What happens before and after ICSI?
ICSI is not a separate treatment from IVF. It is one of the fertilization methods used in the lab during an IVF cycle.
Most ICSI IVF cycles include:
- Ovarian stimulation with injectable gonadotropins
- Monitoring with ultrasound and bloodwork
- Fertilization via ICSI (or conventional insemination)
- Embryo transfer or embryo freezing for a later frozen embryo transfer
When is ICSI recommended?
ICSI is most strongly indicated when fertilization is less likely to occur with conventional insemination, especially in male factor infertility.
CNY Fertility clinical perspective:
In addition to these traditional indications, CNY Fertility uses ICSI as the standard fertilization method in the vast majority of IVF cycles. This approach reflects a clinical priority to minimize the risk of failed fertilization, which can occur even in cycles without obvious male factor infertility.
Because the procedural risks of ICSI are small and fertilization failure can be emotionally and financially devastating, CNY’s default approach favors consistency and fertilization reliability.
At-a-glance: common indications for ICSI
|
Indication |
Why ICSI helps |
Common scenarios |
|
Moderate to severe male factor infertility |
Bypasses sperm’s need to penetrate the egg on its own |
Low sperm count, low motility, poor morphology on semen analysis. |
|
Surgically retrieved sperm |
Maximizes fertilization potential when sperm quantity/motility is limited |
After vasectomy, obstructive azoospermia, testicular/epididymal sperm retrieval[retrieval [references link=”https://www.reproductivefacts.org/news-and-publications/fact-sheets-and-infographics/intracytoplasmic-sperm-injection-icsi/” text=”ASRM ReproductiveFacts: Intracytoplasmic Sperm Injection (ICSI)”] |
|
Prior fertilization failure or very low fertilization |
Reduces the risk of repeating failed fertilization |
Previous IVF cycle with poor fertilization despite mature eggs[eggs [references link=”https://www.reproductivefacts.org/news-and-publications/fact-sheets-and-infographics/intracytoplasmic-sperm-injection-icsi/” text=”ASRM ReproductiveFacts: Intracytoplasmic Sperm Injection (ICSI)”] |
|
Preimplantation genetic testing (PGT) |
Often used to reduce the chance of contamination from extra sperm |
PGT-A/PGT-M/PGT-SR cycles in many labs[labs [references link=”https://www.asrm.org/practice-guidance/practice-committee-documents/intracytoplasmic-sperm-injection-icsi-for-non-male-factor-infertility-a-committee-opinion-2020/” text=”ASRM Committee Opinion: ICSI for non-male factor infertility (2020)”] |
|
Previously cryopreserved (frozen) eggs |
Can bypass barriers to fertilization that may occur after freezing/thawing |
IVF with vitrified oocytes, particularly when conventional insemination is a concern |
Why CNY Fertility uses ICSI as the standard of care
Large studies show that routine ICSI does not consistently improve clinical pregnancy or live birth rates compared with conventional insemination in patients without male factor infertility. However, these same studies also show that ICSI does not reduce pregnancy or live birth rates.
At CNY Fertility, our clinical philosophy prioritizes minimizing the risk of failed fertilization. Because ICSI significantly reduces the likelihood that otherwise healthy eggs will fail to fertilize, and because the procedure itself does not appear to negatively impact pregnancy or live birth outcomes, it is used as the standard fertilization method in IVF care.
Unlike many clinics, CNY does not charge an additional fee for ICSI in self-pay IVF cycles. This allows ICSI to be offered as the standard of care based on risk–benefit considerations rather than cost. As a result, over 99% of IVF cycles at CNY Fertility use ICSI for fertilization.
When conventional IVF insemination may be sufficient
In patients without male factor infertility, large studies and randomized trials show that ICSI does not consistently improve clinical pregnancy or live birth rates compared with conventional IVF insemination.
Importantly, these studies also show that ICSI does not result in lower pregnancy or live birth rates compared with conventional insemination. This means that while ICSI may not improve outcomes in every patient group, it generally does not cause harm when used broadly.
This balance, similar downstream outcomes with a lower risk of fertilization failure, is why fertilization strategies vary across clinics and why some programs, including CNY Fertility, choose to default to ICSI as a standard laboratory approach.
Success rates: ICSI fertilization vs pregnancy outcomes
A common point of confusion is the difference between:
- Fertilization rate
- Clinical pregnancy rate
- Live birth rate
ICSI often achieves high fertilization rates. While higher fertilization does not automatically translate into higher live birth rates in all patient populations, evidence shows that ICSI does not reduce pregnancy or live birth outcomes compared with conventional IVF insemination.
For many clinics, this “no harm” profile, combined with more consistent fertilization, supports the use of ICSI across a wide range of IVF cases.
Does ICSI guarantee fertilization?
No. Even with a technically perfect injection, fertilization can fail due to sperm decondensation (“open up inside the egg”) problems or egg quality limitations.
Risks and limitations of ICSI
ICSI is widely considered a safe, established IVF laboratory technique, but it has some limitations.
Key limitations (why fertilization can still fail)
- Egg activation failure: sometimes the egg does not initiate the intracellular steps needed to fertilize after injection.
- Oocyte quality limitations: poor egg quality (often related to age or ovarian factors) can limit survival, fertilization, and embryo development even with ICSI.
- Sperm decondensation problems: in some cases, sperm DNA may not properly decondense inside the egg, contributing to abnormal or failed fertilization.
- Sperm DNA integrity issues: ICSI can help achieve fertilization when sperm cannot penetrate the egg, but it does not automatically “repair” underlying sperm DNA damage (which can still affect embryo development).
Safety and child outcomes
The procedure itself is considered safe, and discussions about child outcomes focus on small absolute risks and the possibility that some risks relate to underlying infertility factors (including genetic contributors to male factor infertility) rather than ICSI alone.
ICSI is widely considered a safe, established IVF laboratory technique. Safety discussions usually focus on two areas:
1. Procedure-related risks to eggs and embryos
Any micromanipulation can stress eggs, and not every injected egg will survive or fertilize, especially when egg quality is poor.
2. Health outcomes in children conceived with ICSI
ASRM notes that major birth defects occur in about 1.5% to 3% of naturally conceived pregnancies and that certain rare conditions have been associated with ICSI, though the absolute risks remain low. ASRM also emphasizes that some risks may relate to underlying infertility factors (including genetic contributors to male factor infertility) rather than ICSI alone.
Cost of ICSI: national ranges vs CNY Fertility
Many clinics bill ICSI as an add-on to IVF. At CNY Fertility, ICSI is included for self-pay patients as part of their comprehensive IVF packages.
|
Service |
National Average |
CNY Fertility |
Notes |
|
ICSI |
$1,500 |
Included |
Standard at CNY |
FAQ: ICSI
What is ICSI?
ICSI is a lab fertilization method in IVF where one sperm is injected directly into one mature egg to help fertilization occur.
What is ICSI IVF?
“ICSI IVF” usually means an IVF cycle where ICSI (rather than conventional insemination) is used to fertilize the eggs.
What is the ICSI procedure like?
An embryologist prepares mature eggs, selects sperm, and injects a single sperm into each mature egg using micromanipulation tools under a microscope.
Is ICSI better than conventional IVF Fertilization?
ICSI is not “better” across the board. It is most helpful when fertilization is unlikely with conventional insemination (especially male factor infertility). In non-male factor infertility, routine ICSI has not consistently improved live birth outcomes over conventional IVF, but does not seem to harm them either.
ICSI: The takeaway
ICSI is a powerful IVF laboratory tool that makes fertilization possible when sperm cannot reliably fertilize an egg on its own. While large studies show that ICSI does not universally increase live birth rates in all patient groups, evidence also shows that it does not lower pregnancy or live birth outcomes.
At CNY Fertility, this balance, high fertilization reliability with no demonstrated harm to downstream outcomes, is why ICSI is used as the standard of care and included in IVF treatment without additional cost. Individualized decision-making with your fertility team remains essential, but for many patients, ICSI offers consistency and reassurance during an already complex process.