Mini IVF
Mini, Minature, Micro, Low Stimulation, In Vitro Fertilization. They’re the same thing. IVF that uses a reduced stimulation (gonadotropin) medication protocol.
What is Mini IVF?
Mini IVF is In Vitro Fertilization with a reduced or minimal stimulation protocol. You may see terms like mini, miniature, micro, low stim/stimulation, or even natural (though natural IVF is slightly different) to describe the treatment because there is no industry standard terminology. That is because in truth it’s really just IVF. In fact, there is not even a standard mini IVF protocol.
By using fewer medications, one is usually able to produce a small number of high-quality eggs while at the same time being easier on the body and reducing the risk of hyperstimulation to virtually zero (which can also be done by using lupron as a trigger). While some claim that these fewer eggs are higher quality than eggs produced with a standard protocol, there simply isn’t evidence to back this up. Still, Mini IVF can be a good option for many people.
Top Reasons to Do Mini IVF
-
Low or Diminished Ovarian Reserve
Women with DOR may not respond well to the stimulating medications, so taking fewer medications doesn’t mean fewer eggs. Since you wouldn’t be getting any more eggs by taking more medications, there would be little point in doing so. In this case, a mini IVF generally means similar number of eggs, less money, and a reduced risk of hyperstimulation.
-
High Risk of Ovarian Hyperstimulation
Those at risk for OHSS like those with Polycystic Ovarian Syndrome (PCOS) may be a good candidate for Mini IVF since by lowering the amount of medications used, one lowers the risk of hyperstimulating the ovaries and can still produce sufficient egg quantities.
-
Cost
Because fewer medications will be used, the cost of Mini IVF will be substantially less for a single cycle (as medications make up a very significant portion of the total cost of IVF). Know, however, by taking fewer medications it is likely fewer embryos will be made. This means you may have to do another more costly IVF cycle rather than using your remaining frozen embryos for an affordable FET (FETs within one year of your IVF cycle are only $650). That could make mini IVF more expensive in the long run.
-
Philosophy
Some feel that this treatment protocol is more in line with their philosophical beliefs as it reduces the risk of ovarian hyperstimulation as well as reduces the chance of having a large number of remaining embryos after attaining a clinical pregnancy. While there are many suitable options to dealing with these remaining embryos including storing them for the future, discarding them, and our favorite at CNY, embryo donation, many would prefer not to have to make this choice at all.
Other Reasons
Of course, mini IVF is a suitable option for a wide range of people and maybe considered by most people after failing other less intrusive treatments like IUI or for those that have male or female fertility testing that shows those lesser treatment options are not medically advised.
Mini IVF Protocol
Just as there is no standard name for a “mini” IVF cycle, there is no standard protocol for mini or low stim in vitro fertilization cycle. Generally speaking, mini IVF uses a combination of both oral medications (like letrozole, or by some – but generally not recommended by CNY Clomid) and injectable FSH medications. While a conventional IVF cycle often only uses only Injectable medications during the stimulation phase of the IVF cycle, it uses much higher doses than mini IVF.
A mini IVF cycle here at CNY generally uses oral medications for 5 days and a much lower dose of injectable medications for 10 days.
What's the Difference
Conventional IVF Vs. Mini IVF
The key difference between IVF and Mini IVF is the amount of medications used in the simulation protocol and the consequences of the reduced medication. Generally speaking, a mini IVF cycle produces fewer eggs than a full stimulation cycle. Besides those small differences, the process of Mini IVF is virtually the same as IVF.
Mini IVF Process
A Mini IVF cycle still consists of follicular/egg development, egg and sperm retrieval and preparation, fertilization & embryo development, and the embryo transfer.
-
Mini IVF Step 1
Ovarian Stimulation
During ovarian stimulation for a mini IVF cycle, all women will take hormone-based medications that encourage the ovaries to develop a small number of high-quality eggs (as opposed to the usual one egg that is produced each month).
Most women use a small amount of oral stimulation medications like Letrozole (for 5 days) along with a small amount of injectable medications like Gonal F, Follistim, or Menopur (for 10 days).
The stimulation phase of a mini IVF cycle typically begins on days 2-4 of the woman’s cycle.
The entire stimulation phase will start with a baseline appointment to measure hormonal and follicular baseline and will be followed closely with monitoring appointments every few days to track uterine lining, follicular, and hormonal development.
Once the follicles reach the appropriate size, another medication will be used to promote the final maturation of the eggs and properly time the egg retrieval.
-
Mini IVF Step 2
Egg Retrieval & Sperm Retrieval/Collection
The Egg Retrieval is the most significant procedure in a mini IVF cycle. It is a minor outpatient procedure done to collect the developed eggs from the woman’s ovaries and is performed 35 hours after the “trigger,” medication. During the egg retrieval, the physician uses a tiny hollow needle with suction capabilities to collect the eggs from the follicles.
Sperm can be collected through ejaculation into a sterile cup the morning of the egg retrieval, frozen at our office ahead of time, frozen at another location and shipped to ours, purchased from a donor, or collected using more advanced sperm retrieval procedures like a PESA, TESA, or TESE.
Once the sperm is processed, the remaining motile concentrated sperm will be taken to the embryology lab for fertilization.
-
Mini IVF Step 3
Fertilization & Embryo Development
Similar to conventional IVF the eggs may be fertilized via one of two primary methods.
- Conventional Fertilization places sperm in a petri dish and lets fertilization happen by the sperms natural propulsion and penetration into the egg.
- ICSI Fertilization takes an individual sperm and using a tiny hollow needle injects it into the egg
After the egg is fertilized the resulting embryos will grow in nourishing media that mimics the internal environment of a fallopian tube for 2-7 (usually 3-5).
If an embryo is grown to a blastocyst stage (usually day 5), it can then be genetically tested which can be helpful for those at risk of aneuploidy (usually advanced maternal age), those with or carriers of known genetic disorders, of those looking to choose the sex of their child.
-
Mini IVF Step 4
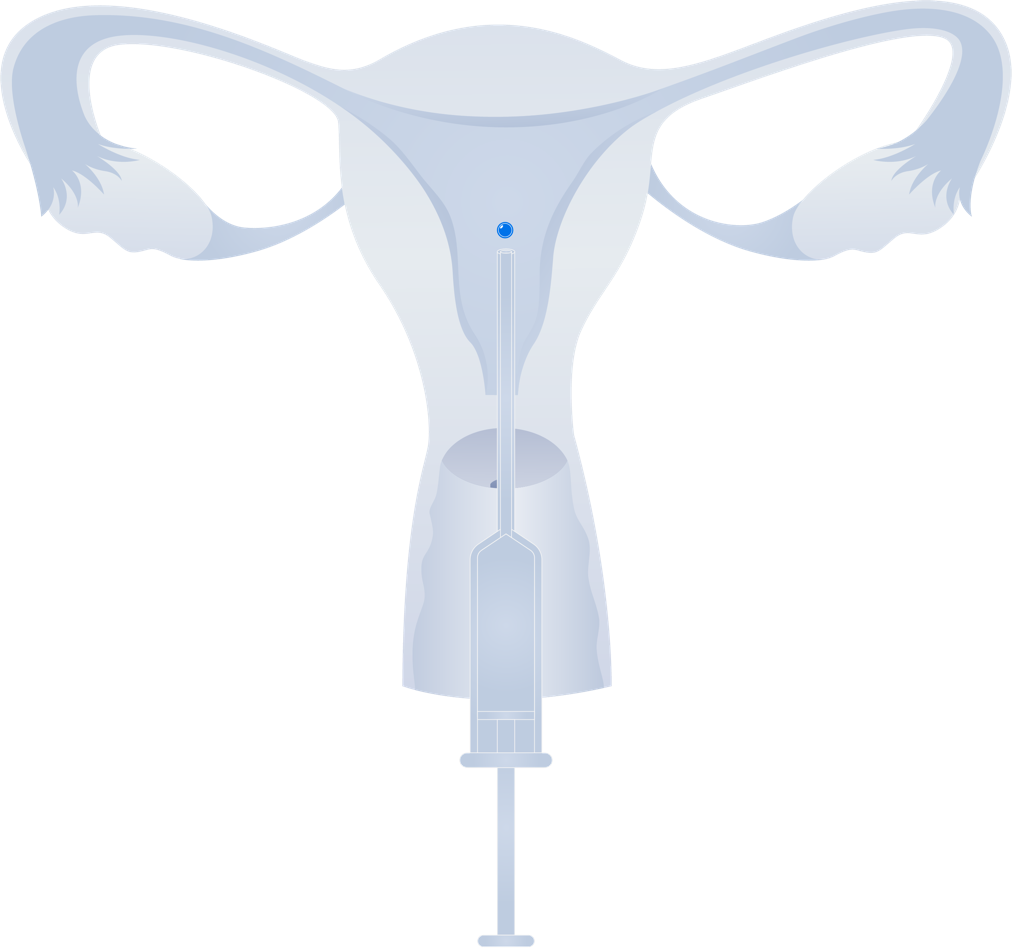
Embryo Transfer
After the early embryonic development, one or two embryo(s) is/are transferred back into the woman’s uterus to continue hopefully implant and continue its develops. An embryo transfer is a very simple “procedure” similar to an IUI, only it is embryos, not sperm, that are loaded into a catheter, gently inserted past the cervix and offloaded into the uterus. If the embryo sticks, pregnancy results.
Though significantly less likely when compared to a standard IVF cycle, any remaining embryos that are not transferred can be frozen and used for a subsequent Frozen Embryo Transfers.
-
Mini IVF Cost
The cost of mini in vitro fertilization is often quoted at a much more affordable price than standard IVF. While it is true the total treatment cost for a single mini cycle is generally less than the average cost of IVF, it’s important to remember two things.
- The fertility clinic charges the same for standard and mini IVF. The cost savings are found in the pharmacy bill and due to the reduced medication protocol.
- While the cost of a single mini IVF cycle is less, it may not be cost-effective in the long run for some. That is because standard IVF protocols often produce more mature embryos that can be frozen for a future FET (as opposed to paying for an entirely new IVF cycle).
The cost of a mini-cycle here at CNY Fertility is $3,999, plus the cost of monitoring, and medications.